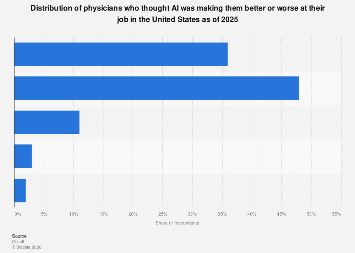
The integration of artificial intelligence (AI) into the medical profession is poised to dramatically reshape the daily operations and performance of physicians across the United States by 2025. While the precise scope and speed of this transformation remain subjects of ongoing analysis and debate, emerging trends and expert projections indicate a significant uplift in efficiency, diagnostic accuracy, and administrative burden reduction. This technological wave is not merely about automating tasks; it represents a fundamental shift in how medical knowledge is leveraged and how patient care is delivered.
The immediate impact of AI on physician job performance is expected to manifest in several key areas. Foremost among these is the enhancement of diagnostic capabilities. AI algorithms, particularly those employing deep learning, have demonstrated remarkable proficiency in analyzing complex medical imagery, such as X-rays, CT scans, and MRIs, often identifying subtle anomalies that might escape the human eye. For instance, AI systems are being trained to detect early signs of diabetic retinopathy, various forms of cancer, and neurological disorders with an accuracy rate that, in some controlled studies, rivals or even surpasses that of experienced radiologists and pathologists. This augmentation of diagnostic power allows physicians to arrive at more precise diagnoses faster, leading to earlier intervention and improved patient outcomes.
Beyond diagnostics, AI’s role in streamlining clinical workflows is anticipated to be substantial. The administrative burden on physicians is a well-documented concern in the U.S. healthcare system, contributing to burnout and diverting valuable time away from patient interaction. AI-powered tools can automate a significant portion of these tasks. Electronic health record (EHR) systems, already a cornerstone of modern medical practice, are increasingly being augmented with AI features for intelligent data entry, summarization of patient histories, and even automated generation of clinical notes. This could free up physicians from hours of paperwork each week, allowing them to focus more intensely on clinical decision-making and direct patient care.
Furthermore, AI is expected to play a crucial role in personalized medicine. By analyzing vast datasets encompassing genomic information, lifestyle factors, and treatment responses from large patient populations, AI can help physicians tailor treatment plans to individual patients with unprecedented precision. This predictive analytics capability can identify patients at higher risk for certain diseases or those who are likely to respond best to specific therapies, moving healthcare away from a one-size-fits-all approach towards highly individualized interventions. The potential for AI to identify optimal drug dosages, predict adverse drug reactions, and suggest the most effective treatment pathways based on a patient’s unique biological profile is immense.
The economic implications of this AI-driven transformation are multifaceted. For healthcare providers, increased efficiency and improved diagnostic accuracy can translate into reduced costs associated with misdiagnosis, prolonged treatment, and unnecessary procedures. A more efficient physician workforce, unburdened by excessive administrative tasks, can potentially see a higher patient throughput, leading to greater revenue generation. However, the initial investment in AI technologies, including software, hardware, and training, represents a significant capital expenditure for healthcare institutions. The return on investment will depend on the successful integration and widespread adoption of these tools.
Globally, the U.S. is not alone in this technological pursuit. Countries like the United Kingdom, Germany, and Canada are also heavily investing in AI for healthcare, driven by similar goals of improving patient care and managing costs. However, the U.S. healthcare market, with its complex payer landscape and high per capita spending, presents a unique environment for AI adoption. The competitive pressures among healthcare systems and the growing demand for value-based care are likely to accelerate the implementation of AI solutions that can demonstrably improve quality and reduce expenditure.
Market data suggests a robust growth trajectory for AI in healthcare. Projections from various market research firms indicate that the global AI in healthcare market, valued in the tens of billions of dollars, is expected to grow at a compound annual growth rate (CAGR) of over 30% in the coming years, with North America, particularly the U.S., being a dominant region. This growth is fueled by increasing data availability, advancements in AI algorithms, and a growing acceptance of AI among healthcare professionals and patients alike.
Expert opinions highlight the collaborative nature of AI in medicine. Dr. Anya Sharma, a leading researcher in medical informatics, notes, "AI is not intended to replace physicians, but rather to augment their abilities. Think of it as an incredibly powerful co-pilot. It can process information at speeds and scales far beyond human capacity, providing insights that empower physicians to make better, more informed decisions." This perspective is crucial; the emphasis is on human-AI synergy, where the physician’s clinical judgment, empathy, and understanding of the patient’s broader context remain paramount.
However, challenges remain. Ethical considerations surrounding data privacy, algorithmic bias, and accountability in AI-driven medical decisions are critical areas that require careful navigation. Ensuring that AI systems are trained on diverse datasets to avoid perpetuating existing health disparities is paramount. Furthermore, the successful integration of AI requires comprehensive training and upskilling of the healthcare workforce. Physicians will need to develop new competencies to effectively utilize and interpret AI-generated insights.
The regulatory landscape also plays a significant role. As AI tools become more sophisticated and integrated into clinical practice, regulatory bodies like the Food and Drug Administration (FDA) are actively developing frameworks to ensure the safety and efficacy of these technologies. Clear guidelines and approval processes are essential for fostering trust and facilitating widespread adoption.
Looking towards 2025, the envisioned impact of AI on U.S. physicians is one of enhanced capabilities and reduced operational friction. Physicians will likely spend less time on repetitive tasks and more time on complex problem-solving, patient engagement, and strategic care planning. The diagnostic accuracy will improve, leading to better patient outcomes and potentially a reduction in costly medical errors. The economic benefits, while requiring initial investment, are expected to materialize through increased efficiency and optimized resource allocation within the healthcare system. The journey of AI integration is ongoing, but its trajectory by 2025 promises a significantly more advanced and effective medical profession.