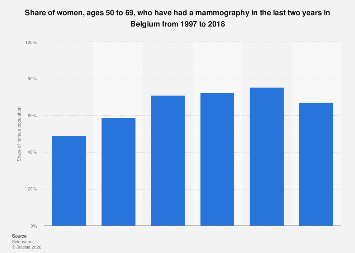
In Belgium, the landscape of preventative healthcare for women over the age of 50 is prominently shaped by mammography screening programs, a critical tool in the early detection of breast cancer. While specific, granular data on participation rates often resides within premium datasets requiring subscription access, the broader context of these screening initiatives points to significant public health objectives and, by extension, economic considerations. These programs are not merely a clinical intervention; they represent a substantial investment in national well-being, with far-reaching implications for healthcare expenditure, workforce productivity, and the overall economic vitality of the nation. Understanding the participation and efficacy of these programs is paramount for policymakers, healthcare providers, and the public alike.
Breast cancer remains a leading cause of cancer-related mortality among women globally, and early detection through regular mammography screening has been unequivocally demonstrated to improve survival rates and reduce the need for more aggressive and costly treatments. Belgium, like many developed European nations, has established organized screening programs designed to reach its target demographic. These programs typically involve inviting women within a specific age bracket, often between 50 and 69 years old, for regular mammograms, usually every two years. The aim is to identify abnormalities at their earliest, most treatable stages, thereby mitigating the disease’s progression and its associated human and economic toll.
The effectiveness of such screening programs is intrinsically linked to participation rates. A high uptake ensures that a significant portion of the at-risk population benefits from the early detection potential. Conversely, lower participation rates can lead to a higher proportion of cancers being diagnosed at later, more advanced stages, which often translates to poorer prognoses and more complex, expensive treatment regimens. Factors influencing participation are multifaceted, encompassing awareness levels, access to healthcare facilities, cultural attitudes towards health screenings, socioeconomic status, and the perceived efficacy and convenience of the screening process itself. In Belgium, public health campaigns and accessible screening centers are key pillars in encouraging women to engage with these vital health checks.
The economic ramifications of effective mammography screening are substantial and often underestimated. Early detection can significantly reduce the average cost of breast cancer treatment. When cancer is caught early, less invasive surgical procedures, shorter courses of chemotherapy or radiation, and fewer long-term supportive care needs are typically required. This translates into direct savings for the national healthcare system, which is often funded through a combination of public and private insurance. Furthermore, by enabling women to remain healthy and active for longer, early detection contributes to sustained workforce participation. This preserves valuable human capital and reduces the economic burden associated with long-term disability and premature retirement due to illness.
Conversely, delayed diagnosis can lead to a cascade of escalating healthcare costs. Advanced breast cancer often necessitates more aggressive surgical interventions, including mastectomy and reconstructive surgery, prolonged and intensive chemotherapy and radiation therapies, and potentially costly targeted therapies or immunotherapy. The psychological and physical toll on patients also leads to increased demand for palliative care, mental health support, and long-term rehabilitation services. The economic impact extends beyond direct medical costs, encompassing lost productivity due to extended periods of illness, absenteeism from work, and the caregiving responsibilities placed on family members.
Globally, mammography screening practices and their associated participation rates vary considerably. Countries with robust, well-funded national health services and proactive public health strategies generally exhibit higher screening uptake. For instance, countries like the United Kingdom and Canada, with their universal healthcare systems, have historically prioritized organized screening programs. In contrast, countries with more fragmented healthcare systems or significant disparities in access may face greater challenges in achieving widespread coverage. Benchmarking Belgium’s screening rates against these international peers provides valuable insights into areas of strength and potential improvement.
The statistical data concerning mammography screening in Belgium, while not publicly detailed in its entirety, forms a crucial component of public health surveillance. Understanding the percentage of eligible women who undergo screening, the detection rates of various stages of breast cancer, and the subsequent outcomes is essential for evaluating the return on investment for these public health initiatives. These metrics inform budget allocations, guide the development of targeted outreach programs to underserved populations, and help refine screening protocols to maximize their effectiveness.
The Belgian healthcare system, like many in Europe, operates under the principle of solidarity, where the costs of healthcare are distributed across the population. Investments in preventative measures like mammography screening are therefore viewed not just as an expenditure but as a strategic allocation of resources aimed at reducing the overall burden of disease. The long-term economic benefits of a healthier population, including reduced healthcare spending and increased economic productivity, are a compelling argument for continued and potentially enhanced support for these screening programs.
Moreover, the technological advancements in mammography, such as digital mammography and tomosynthesis (3D mammography), offer improved accuracy in detecting abnormalities and reducing false positives and negatives. The adoption and accessibility of these advanced technologies within Belgium’s screening programs can further enhance their efficacy and patient experience, potentially boosting participation rates. The cost-effectiveness of these newer technologies in the context of early detection and reduced downstream treatment costs is a continuous area of research and policy consideration.
In conclusion, while precise statistical figures for mammography screening participation among Belgian women over 50 may require specialized access, the strategic importance of these programs is undeniable. They are cornerstones of preventative healthcare, directly impacting breast cancer survival rates and significantly influencing the economic landscape through reduced treatment costs and sustained workforce participation. As Belgium continues to prioritize the health and well-being of its citizens, ongoing investment in and evaluation of its mammography screening initiatives will remain critical for achieving both public health and economic prosperity. The commitment to early detection is a prudent, long-term strategy that benefits individuals, families, and the nation as a whole.