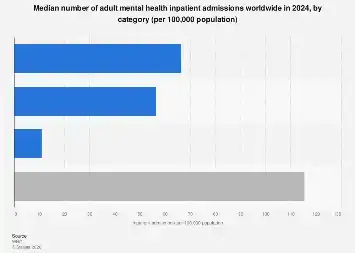
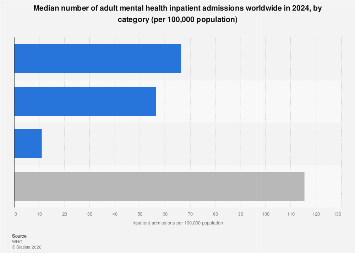
The global landscape of mental health treatment saw a median of 105 adult inpatient admissions per 100,000 population in 2024, indicating a significant demand for acute psychiatric care across diverse healthcare systems worldwide. This aggregate figure, however, masks considerable variation in how and where these admissions occur, highlighting distinct approaches to mental healthcare provision and the underlying infrastructure supporting it. The data, compiled and analyzed for 2024, offers a crucial snapshot of the pressures and priorities within global mental health services, with implications for resource allocation, policy development, and the ongoing pursuit of equitable access to care.
Psychiatric hospitals, traditionally the cornerstone of inpatient mental health treatment, accounted for the largest proportion of these admissions, with a global median of 60 admissions per 100,000 population. This figure underscores the continued reliance on specialized, freestanding institutions for managing severe and persistent mental health conditions requiring intensive, round-the-clock care. The operation of such facilities involves substantial investment in specialized staff, including psychiatrists, psychologists, psychiatric nurses, and social workers, as well as the maintenance of secure and therapeutic environments. Global expenditure on mental health services varies widely, but the significant number of admissions to psychiatric hospitals suggests a persistent need for these dedicated care settings, particularly in regions where community-based mental health infrastructure may be less developed or overburdened.
Following closely, psychiatric units within general hospitals represented another major channel for inpatient mental health care, with a median of 35 admissions per 100,000 population. This model of care integration offers potential benefits, including easier access to broader medical services for patients with co-occurring physical health issues and the destigmatization of mental illness by embedding psychiatric care within general healthcare settings. The presence of dedicated psychiatric wards in general hospitals can also facilitate more seamless transitions between acute inpatient care and subsequent outpatient follow-up within the same healthcare network. The growth and development of these integrated units are often influenced by national healthcare reforms and funding models that encourage multidisciplinary approaches and the deinstitutionalization of mental health services, aiming to bring care closer to the patient’s community.
A notably lower median admission rate of 10 per 100,000 population was observed for mental health community residential facilities. These facilities typically offer longer-term support and rehabilitation for individuals with chronic mental health conditions, focusing on developing independent living skills and social reintegration. The lower admission rate to these settings, compared to more acute care facilities, could reflect a number of factors. It may indicate a greater emphasis on early intervention and community-based support services that prevent the need for residential care, or it could point to limitations in the availability or accessibility of these specialized residential programs in certain regions. Furthermore, the philosophy of care in these facilities often prioritizes gradual rehabilitation and stepped-down care, meaning individuals may spend longer periods in these settings, thus potentially impacting annual admission figures.
The disparity in admission rates across these different care modalities suggests a complex global picture of mental health service delivery. In developed economies, there is often a push towards community-based care and the reduction of long-stay inpatient facilities, a trend driven by the recognition of the therapeutic benefits of social integration and the economic efficiencies of preventing acute relapses. However, the persistent high volume of admissions to psychiatric hospitals globally indicates that for a significant portion of the population, intensive inpatient treatment remains indispensable. This can be attributed to the severity of certain mental illnesses, the lack of robust community support networks, or the limited capacity of outpatient services to manage complex cases.
The economic implications of these admission patterns are profound. The cost of inpatient mental health care, particularly in specialized psychiatric hospitals, is substantial, encompassing staffing, infrastructure, medication, and therapeutic interventions. High admission rates translate directly into significant public and private healthcare expenditure. Conversely, investments in robust community-based mental health services, while requiring upfront capital, can potentially yield long-term economic benefits by reducing the need for costly hospitalizations, improving workforce participation for individuals with mental health conditions, and decreasing the societal burden associated with untreated or inadequately treated mental illness.
Global comparisons further illuminate these trends. Countries with well-funded and comprehensive mental health systems, often characterized by strong primary care integration and extensive community support networks, may exhibit lower rates of inpatient admissions to psychiatric hospitals and higher utilization of community residential facilities. Conversely, nations with more limited resources or fragmented healthcare systems might see a greater reliance on traditional psychiatric hospitals. The World Health Organization (WHO) consistently advocates for increased investment in mental health, emphasizing the need to shift resources towards prevention, early intervention, and community-based care models to improve outcomes and achieve better economic efficiency.
The COVID-19 pandemic has also had a significant, albeit complex, impact on mental health service utilization globally. While the pandemic led to an increased prevalence of mental health challenges, including anxiety and depression, the immediate impact on inpatient admission rates was varied. Some regions reported initial drops in elective admissions due to healthcare system strain, while others later saw surges as the mental health consequences of isolation, economic hardship, and grief became more pronounced. The 2024 data provides a contemporary view of how these systems are adapting and responding to ongoing mental health needs in the post-pandemic era.
Understanding these global admission trends is critical for policymakers, healthcare providers, and researchers. It informs decisions about where to allocate resources, how to structure mental health services for optimal patient outcomes, and how to foster a more integrated and accessible mental healthcare system worldwide. The continued reliance on psychiatric hospitals, alongside the growing role of general hospital units and community residential facilities, paints a picture of a multifaceted approach to mental health, one that is continually evolving in response to clinical evidence, economic realities, and societal priorities. As global mental health needs continue to grow, the data from 2024 serves as a vital benchmark for progress and a call to action for sustained innovation and investment in mental healthcare for all.