Colorectal cancer (CRC) continues to present a significant public health challenge across the European Union, with notable variations in incidence rates observed among its member states and between male and female populations. As of 2024, preliminary data indicates a stark gender disparity, with men generally facing a higher likelihood of developing the disease. While specific figures for the overall EU incidence rate remain proprietary, the available data points to a substantial public health burden that necessitates ongoing surveillance, research, and targeted intervention strategies.
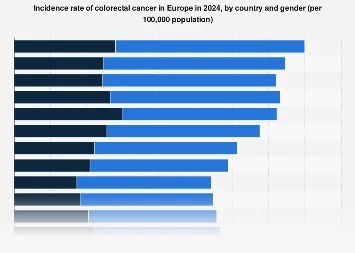
Analysis of country-specific data reveals a compelling geographical distribution of CRC incidence. Hungary emerges as a nation with a particularly high burden, reporting the most elevated incidence rates for men in 2024. This finding is concerning and suggests a potential confluence of genetic predispositions, lifestyle factors, environmental exposures, and healthcare system characteristics that warrant in-depth investigation. Conversely, Austria stands out with the lowest reported incidence rates for men within the EU. This contrast between the two nations highlights the complex interplay of factors influencing cancer development and underscores the importance of comparative epidemiology in identifying best practices and areas for improvement.
The gender dimension of colorectal cancer incidence within the EU is equally pronounced. For women, Hungary also registers the highest incidence rates, mirroring the trend observed in the male population. This suggests that certain underlying factors may be disproportionately affecting both sexes within specific national contexts, or that common risk factors are at play with differing levels of impact. In contrast, Austria demonstrates the lowest incidence rates for women as well, reinforcing its position as an outlier with a comparatively lower burden of the disease among its female populace.
These figures, presented as age-standardized rates per 100,000 population, are crucial for understanding the true epidemiological burden. The age-standardization process, using the European 2013 population as a standard, ensures that comparisons between countries are not skewed by differences in their demographic structures. This method allows for a more accurate assessment of inherent risks within populations, isolating the impact of cancer incidence from age-related variations.
The economic implications of colorectal cancer incidence across the EU are substantial. Beyond the direct healthcare costs associated with diagnosis, treatment, and palliative care, there are significant indirect economic consequences. These include lost productivity due to illness, premature mortality, and the burden on caregivers. For nations with higher incidence rates, the strain on national health budgets and social security systems can be considerable. Conversely, countries with lower rates may benefit from a healthier, more productive workforce and reduced healthcare expenditures related to this specific cancer.
Understanding the drivers behind these geographical and gender-based disparities is paramount. While lifestyle factors such as diet, physical activity, alcohol consumption, and smoking are well-established contributors to CRC risk, their prevalence and impact can vary significantly across Europe. For instance, dietary patterns rich in red and processed meats, coupled with low fiber intake, have been linked to increased risk. Similarly, sedentary lifestyles and obesity rates, which differ considerably across EU countries, play a critical role. Socioeconomic factors also contribute, with disparities in access to early screening, diagnostic services, and quality healthcare potentially exacerbating incidence rates in certain regions or demographic groups.
The European Union, through initiatives like Europe’s Beating Cancer Plan, is actively working to address the cancer burden. This plan emphasizes prevention, early detection, and improved treatment outcomes. The identification of countries with high incidence rates, such as Hungary, provides crucial data for targeted public health interventions. This could involve intensified screening programs, public awareness campaigns focused on risk factors and early symptoms, and research into specific genetic or environmental factors prevalent in those regions.
Conversely, the low incidence rates observed in countries like Austria offer valuable insights into potential protective factors. Further research into the lifestyle, environmental, and healthcare system characteristics of these nations could yield transferable strategies for other EU member states. This might include examining the effectiveness of their screening protocols, the widespread adoption of healthy lifestyle choices, or the impact of specific public health policies.
The role of screening programs cannot be overstated. Early detection through regular screening, such as fecal occult blood tests or colonoscopies, significantly improves treatment outcomes and survival rates for colorectal cancer. Variations in the uptake and accessibility of these screening programs across different EU countries could contribute to the observed differences in incidence and mortality. Countries with robust, widely adopted screening initiatives are likely to diagnose the disease at earlier, more treatable stages, which can influence overall incidence statistics and, more importantly, patient prognoses.
Globally, colorectal cancer is a leading cause of cancer-related deaths. When compared to other developed nations outside the EU, the incidence rates within Europe present a mixed picture. Some countries in North America and Oceania also face significant challenges with CRC, while others have made substantial progress through effective public health strategies and advanced medical technologies. The continuous monitoring of global trends and the sharing of best practices are essential for a coordinated international approach to cancer control.
The age-standardized incidence rate is a critical metric, but it represents only one facet of the complex picture of cancer burden. Mortality rates, survival rates, and quality of life for cancer survivors are equally important indicators. While the data presented focuses on incidence, it lays the groundwork for further analysis into the effectiveness of treatment protocols and the overall impact of CRC on European populations.
In conclusion, the 2024 data on colorectal cancer incidence across the EU highlights significant variations by country and gender. Hungary and Austria serve as compelling examples of nations at opposite ends of the spectrum, underscoring the diverse epidemiological landscape within the Union. Addressing this persistent health challenge will require a multi-pronged approach, encompassing robust prevention strategies, accessible and effective screening programs, targeted public health interventions in high-incidence regions, and ongoing research to unravel the complex interplay of genetic, environmental, and lifestyle factors. The economic and social implications are profound, making the reduction of colorectal cancer incidence a critical objective for the European Union’s public health agenda.