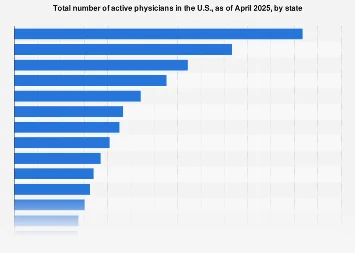
California boasts the nation’s largest contingent of active physicians, with preliminary figures for September 2025 indicating a staggering number of medical professionals within its borders. This concentration, while seemingly a boon for healthcare access in the Golden State, starkly contrasts with the physician scarcity observed in other regions, particularly less populated states like Wyoming, which registers a fraction of California’s medical workforce. This disparity underscores a persistent and complex challenge facing the United States: ensuring equitable distribution of healthcare services and personnel across its diverse geographic and demographic landscape. The sheer volume of doctors in California, estimated to be in the hundreds of thousands, not only reflects its status as the most populous state but also its significant economic capacity to attract and retain medical talent. In contrast, states with smaller populations and often less robust healthcare infrastructure grapple with critical shortages, impacting timely access to care and exacerbating existing health inequities.
The distribution of physicians within California itself, and by extension across the nation, reveals a pronounced specialization trend. The state leads not only in the overall number of doctors but also in the crucial categories of primary care physicians and specialists. This concentration of expertise means that while California may have ample access to a wide range of medical services, other states may face significant limitations, particularly in specialized fields. Nationally, California accounts for a substantial percentage of both primary care and specialist physicians, a figure that underscores its outsized role in the U.S. medical landscape. Following California, New York and Texas emerge as other states with considerable numbers of primary care physicians, vital for the foundational delivery of healthcare. The specialization landscape further illustrates this trend, with psychiatry, surgery, and anesthesiology consistently ranking among the most prevalent medical disciplines. This concentration of specialists, while beneficial for those residing in leading states, can create access barriers in areas where such expertise is scarce, potentially leading to longer wait times, increased travel burdens for patients, and a reliance on more generalized care when specialized attention is required.
Beyond the sheer numbers, the persistent issue of physician burnout casts a long shadow over the healthcare profession, irrespective of state-level physician density. This phenomenon, characterized by emotional exhaustion, depersonalization, and a reduced sense of personal accomplishment, affects a significant portion of the medical workforce. Data reveals a notable gender disparity in burnout rates, with female physicians reporting disproportionately higher levels of exhaustion compared to their male counterparts. This divergence highlights the complex interplay of professional demands, personal responsibilities, and systemic factors that may contribute to burnout, with women often navigating unique challenges. Furthermore, the intensity of specific medical specialties plays a critical role in the prevalence of burnout. Physicians in high-pressure fields such as emergency medicine consistently report the highest rates of burnout, reflecting the demanding nature of their work, the critical decision-making involved, and the often-unpredictable environments they operate within.
The economic implications of this uneven physician distribution and the pervasive issue of burnout are far-reaching. States with fewer physicians often face higher healthcare costs due to increased reliance on emergency services, longer hospital stays, and the necessity of attracting physicians through competitive compensation packages, which can ultimately be passed on to patients. Workforce shortages can also hinder economic development by impacting the ability of communities to attract new businesses and retain residents who prioritize access to quality healthcare. The cost of physician burnout is also substantial, manifesting in decreased productivity, increased medical errors, and higher rates of physician turnover. This attrition not only incurs recruitment and training costs for healthcare institutions but also disrupts continuity of care for patients. Addressing physician burnout requires multifaceted strategies, including workload management, improved administrative support, mental health resources, and fostering a more supportive work environment.
The future of healthcare workforce distribution in the U.S. hinges on a proactive and strategic approach to address these critical issues. Policy initiatives aimed at incentivizing physicians to practice in underserved rural and urban areas, such as loan forgiveness programs, enhanced reimbursement rates, and the expansion of telehealth services, are crucial. Furthermore, fostering a culture that prioritizes physician well-being and actively combats burnout is not merely an ethical imperative but an economic necessity. Investing in physician education and training, particularly in primary care and in specialties facing shortages, will be vital to meeting the evolving healthcare needs of the nation. The data on physician distribution and burnout serves as a clarion call for a comprehensive re-evaluation of how the U.S. cultivates, distributes, and supports its medical professionals, ensuring that quality healthcare is accessible to all Americans, regardless of their geographic location or socioeconomic status. As the nation navigates demographic shifts and an aging population, the demand for physicians is projected to rise, making the equitable distribution and well-being of this vital workforce more critical than ever.