A significant portion of global economic output is being channeled directly from household budgets into healthcare services, underscoring a critical, yet often overlooked, aspect of national economic health and individual financial well-being. This phenomenon, measured as out-of-pocket (OOP) health spending as a share of Gross Domestic Product (GDP), reveals stark disparities across nations and offers a nuanced view of how different countries approach healthcare financing and the resultant economic pressures on their citizens. In many developed economies, robust public health systems and comprehensive insurance coverage significantly buffer individuals from direct medical costs. However, in a substantial number of countries, particularly low- and middle-income nations, households bear a disproportionately large share of healthcare expenses, impacting their disposable income, savings, and overall economic stability.
The implications of high OOP spending are multifaceted, extending beyond individual financial strain to affect broader macroeconomic indicators. When a larger percentage of a nation’s GDP is consumed by direct healthcare payments, it can indicate several underlying issues. It might point to a less developed public healthcare infrastructure, where government investment in health is insufficient to cover essential services. Alternatively, it could signal gaps in social safety nets, leading to a greater reliance on private insurance or direct payments for even basic medical needs. This can create a vicious cycle: high OOP costs can push individuals and families into poverty, reducing their capacity to contribute to the economy through consumption or investment, and potentially leading to a decline in overall productivity due to untreated or inadequately managed health conditions.
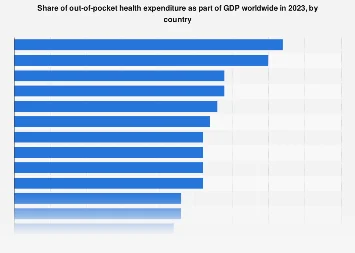
Examining international data reveals a diverse landscape. Countries with highly developed universal healthcare systems, such as those in Scandinavia or parts of Western Europe, typically exhibit very low percentages of GDP dedicated to OOP health spending. For instance, nations like Sweden or Norway, with their comprehensive tax-funded healthcare models, often see OOP expenditures representing less than 1% of their GDP. This allows households to allocate a larger portion of their income towards other goods and services, fostering economic growth and improving quality of life. In contrast, some countries in Sub-Saharan Africa or parts of Southeast Asia, while making strides in healthcare access, still grapple with OOP shares that can exceed 5% or even 10% of their GDP. This indicates a heavy reliance on user fees and private sector provision, placing a considerable burden on citizens who may already be operating with limited financial resources.
The economic impact of these disparities is profound. High OOP spending can act as a significant impediment to poverty reduction efforts. Medical emergencies can quickly deplete savings, forcing families to sell assets, take on high-interest debt, or forgo essential expenditures like education and nutrition. This not only impacts the immediate household but can have generational consequences, perpetuating cycles of disadvantage. Furthermore, it can deter individuals from seeking timely medical attention, leading to poorer health outcomes and increased long-term healthcare costs for the nation as a whole when conditions worsen and require more complex, expensive interventions.
Market data and projections from international organizations like the World Health Organization (WHO) and the World Bank consistently highlight the challenges posed by excessive OOP health spending. These organizations advocate for strengthening public health financing mechanisms, expanding social health insurance coverage, and implementing policies to reduce catastrophic health expenditure for households. The goal is to move towards a more equitable and sustainable healthcare financing model that protects individuals from financial ruin while ensuring access to quality care.
The trend in many middle-income countries is particularly noteworthy. As these economies grow and their populations age, the demand for healthcare services increases. Without commensurate growth in public health funding or effective insurance schemes, OOP spending can rise as a proportion of GDP. This presents a critical policy challenge: balancing economic development with the imperative to provide affordable healthcare. Investing in primary healthcare, preventative services, and robust public health insurance programs are key strategies that can help mitigate this trend and ensure that economic progress translates into improved health and financial security for all citizens.
Global comparisons offer valuable lessons. Countries that have successfully implemented universal health coverage schemes, often through a combination of public funding, mandatory insurance, and regulated private provision, have demonstrated a capacity to keep OOP spending at manageable levels. These systems are designed to pool risk across the entire population, ensuring that the financial burden of illness is shared and that no single individual or family faces insurmountable costs. The success of these models is not merely a matter of social justice; it is also an economic imperative, fostering a healthier, more productive workforce and a more resilient economy.
The pursuit of universal health coverage is, therefore, intrinsically linked to broader economic development strategies. By reducing the financial barriers to accessing healthcare, nations can unlock significant economic potential. A healthier population is a more productive population. Reduced OOP spending can free up household income for investment in education, entrepreneurship, and other economic activities. This, in turn, can drive innovation, create jobs, and foster sustainable economic growth. The challenge lies in designing and implementing financing mechanisms that are both effective in delivering care and equitable in their distribution of costs, ensuring that healthcare is a catalyst for economic progress rather than a barrier.
Furthermore, the digital transformation of healthcare systems, including the adoption of telemedicine, electronic health records, and data analytics, offers new avenues for improving efficiency and reducing costs. These innovations, when coupled with appropriate policy frameworks, can help to streamline service delivery, improve patient outcomes, and potentially lower the overall financial burden on both individuals and the state. However, ensuring equitable access to these digital health solutions is crucial to avoid exacerbating existing inequalities.
In conclusion, the proportion of GDP dedicated to out-of-pocket healthcare expenditure serves as a critical barometer of a nation’s healthcare system’s strength, its social safety net’s effectiveness, and its citizens’ financial resilience. While progress has been made globally in expanding access to healthcare, the persistent burden of OOP spending in many regions demands continued attention and strategic policy interventions. Governments, international organizations, and healthcare providers must collaborate to build robust, equitable, and financially sustainable healthcare systems that protect individuals from catastrophic health costs, thereby fostering not only better health outcomes but also stronger, more resilient economies for the future.