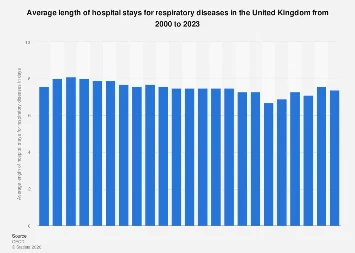
The average duration of hospital stays for respiratory diseases has become a critical metric for healthcare systems globally, reflecting not only patient acuity but also the efficiency of treatment protocols and the broader impact of respiratory conditions on healthcare infrastructure. Recent analyses reveal a complex and evolving picture, with variations across different respiratory ailments and geographical regions, underscoring the persistent challenge posed by lung health. Understanding these trends is paramount for policymakers, healthcare providers, and researchers aiming to optimize resource allocation, improve patient outcomes, and mitigate the economic burden associated with respiratory illnesses.
Globally, the management of respiratory conditions accounts for a significant portion of hospital bed utilization and expenditure. While specific data points on average lengths of stay can fluctuate based on data collection methodologies, the underlying drivers of these durations offer valuable insights. Factors such as the severity of the infection, the presence of comorbidities, the effectiveness of early intervention, and the availability of advanced respiratory support technologies all play a role. For instance, severe cases of pneumonia, acute exacerbations of Chronic Obstructive Pulmonary Disease (COPD), and advanced stages of lung cancer often necessitate prolonged hospitalizations, involving intensive care, mechanical ventilation, and comprehensive rehabilitation.
The economic implications of these extended stays are substantial. Beyond the direct costs of medical care, including pharmaceuticals, diagnostic tests, and specialized equipment, longer hospitalizations translate into increased labor costs for nursing and medical staff, as well as the potential for reduced hospital capacity, impacting the ability to treat other conditions. Furthermore, extended stays can lead to significant indirect costs for patients and their families, such as lost wages and the need for ongoing care post-discharge. Estimates suggest that respiratory diseases collectively represent billions of dollars in healthcare expenditure annually worldwide, with length of stay being a primary cost driver.
Delving into specific respiratory conditions, the average length of stay can vary considerably. For acute respiratory infections like influenza or bronchitis, hospitalizations are typically shorter, often ranging from a few days to a week, provided there are no complications. However, when these infections lead to secondary bacterial pneumonia or trigger severe exacerbations in individuals with underlying lung conditions, the duration can extend significantly. COPD exacerbations, for example, are a leading cause of hospitalization in many developed countries. While a typical uncomplicated exacerbation might require a 5-7 day stay, severe cases requiring ventilatory support or extensive pulmonary rehabilitation can extend this to two weeks or more.
Asthma, another prevalent respiratory condition, also contributes to hospital admissions. While milder asthma attacks may be managed in outpatient settings, severe exacerbations necessitate hospitalization. The length of stay for asthma can vary, but often falls within a similar range to COPD exacerbations, depending on the response to treatment and the presence of triggers. The economic toll of asthma hospitalizations alone is considerable, driven by emergency room visits, intensive care unit admissions, and prolonged recovery periods.
The impact of chronic lung diseases, such as interstitial lung diseases and cystic fibrosis, on hospital stay lengths is also noteworthy. Patients with these conditions often experience recurrent exacerbations or progressive deterioration, leading to more frequent and prolonged hospitalizations. These longer stays are not only resource-intensive but also indicative of the complex and often unremitting nature of these diseases, highlighting the need for robust outpatient management strategies and home-based care options to reduce the reliance on acute hospital settings.
International comparisons offer a broader perspective on these trends. Developed nations with advanced healthcare systems often have more sophisticated diagnostic tools and treatment protocols, which can potentially lead to shorter hospital stays for certain conditions due to earlier and more effective interventions. However, these systems also tend to have higher overall healthcare expenditures. Conversely, developing nations may face challenges in providing timely and advanced respiratory care, potentially leading to longer hospital stays for preventable or treatable conditions due to resource limitations and delayed diagnoses. The burden of infectious respiratory diseases, such as tuberculosis, also varies significantly by region, with differing lengths of stay influenced by treatment regimens and the prevalence of drug-resistant strains.
The emergence of new respiratory pathogens, as vividly demonstrated by the COVID-19 pandemic, has dramatically reshaped hospitalization patterns and lengths of stay. The severe respiratory distress caused by SARS-CoV-2 often necessitated prolonged stays in intensive care units, requiring mechanical ventilation for extended periods. The average length of stay for severe COVID-19 cases often exceeded two to three weeks, placing immense pressure on healthcare systems worldwide. While vaccination and improved treatment protocols have since led to a reduction in the severity and duration of hospitalizations for many COVID-19 patients, the pandemic’s legacy continues to influence respiratory disease management and preparedness.
Furthermore, the evolving understanding of respiratory physiology and the development of innovative treatments are continuously influencing hospitalization lengths. Advances in non-invasive ventilation, bronchodilator therapies, pulmonary rehabilitation programs, and targeted pharmacotherapies for conditions like COPD and idiopathic pulmonary fibrosis are enabling more effective management outside of acute hospital settings, potentially leading to shorter stays and reduced readmission rates. The focus is increasingly shifting towards integrated care models that emphasize chronic disease management, early detection, and proactive interventions to prevent exacerbations and reduce the need for hospitalization.
The role of public health initiatives and preventive measures cannot be overstated in influencing the overall burden of respiratory diseases and, consequently, hospital stay lengths. Smoking cessation programs, vaccination campaigns against influenza and pneumococcal pneumonia, and public awareness campaigns regarding air quality and respiratory hygiene all contribute to reducing the incidence and severity of respiratory illnesses. A reduction in the overall number of respiratory admissions naturally leads to a decrease in the total number of patient-days spent in hospitals, freeing up resources and reducing healthcare costs.
In conclusion, the average length of hospital stays for respiratory diseases is a dynamic indicator reflecting the complex interplay of disease burden, healthcare system efficiency, technological advancements, and public health strategies. While specific figures may vary, the overarching trend underscores the persistent significance of respiratory health challenges. Continued investment in research, innovation in treatment modalities, and robust public health interventions are crucial for optimizing patient care, managing healthcare resources effectively, and ultimately improving the quality of life for individuals affected by respiratory ailments across the globe. The economic imperative to reduce unnecessary hospitalizations and improve the efficiency of care delivery remains a central theme in the ongoing discourse surrounding respiratory health.