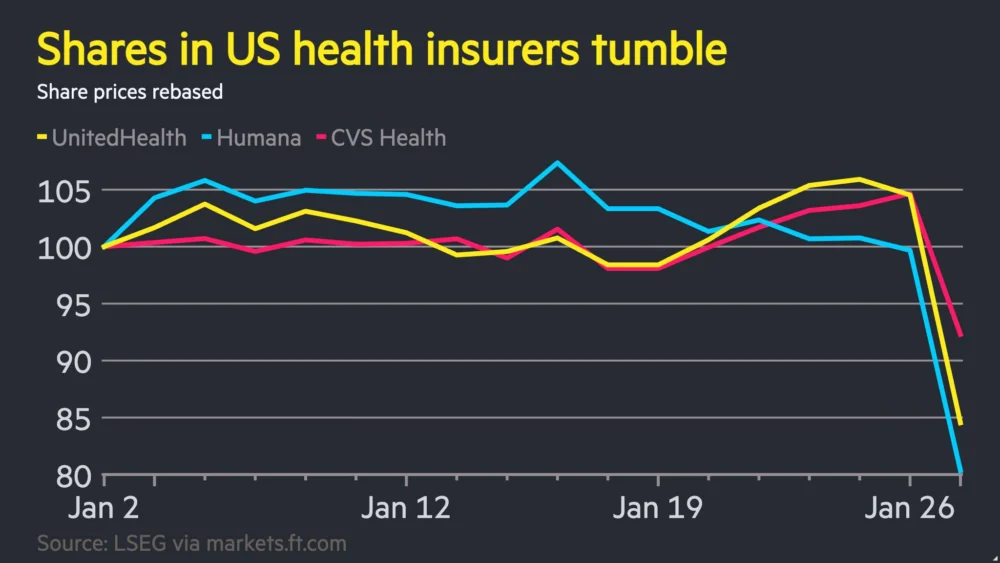
The American healthcare landscape, long a bastion of reliable returns for institutional investors, was sent into a tailspin this week as the incoming administration’s blueprint for Medicare spending sent shockwaves through Wall Street. Shares of the nation’s largest managed-care organizations plummeted following signals that the federal government intends to aggressively recalibrate reimbursement rates and tighten the fiscal leash on Medicare Advantage, the private-sector alternative to traditional Medicare. This sudden pivot in policy direction has erased tens of billions of dollars in market capitalization, forcing a stark re-evaluation of the profitability of the multi-trillion-dollar US healthcare industry.
For the better part of a decade, Medicare Advantage (MA) has been the primary growth engine for giants like UnitedHealth Group, Humana, and CVS Health’s Aetna. These private plans, which are funded by the federal government but administered by private corporations, now cover more than half of all eligible Medicare beneficiaries—roughly 33 million people. However, the proposed spending plan under the Trump administration suggests a departure from the relatively generous payment environment that characterized the previous decade. By targeting what policy advisors describe as "systemic inefficiencies" and "overpayments," the new fiscal strategy threatens the very margins that have made these stocks darlings of the S&P 500.
The market reaction was swift and unforgiving. UnitedHealth Group, the industry bellwether and the largest health insurer by market value, saw its stock price drop by its widest margin in years, dragging down the broader Dow Jones Industrial Average. Humana, which is more heavily leveraged toward the Medicare Advantage market than its diversified peers, suffered an even more precipitous decline, with its shares hitting multi-year lows. The sell-off extended to Elevance Health and Centene, as investors scrambled to price in a future where federal "per-member, per-month" payments may no longer keep pace with the rising costs of medical utilization.
At the heart of the investor panic is the proposed shift in how the Centers for Medicare & Medicaid Services (CMS) will calculate benchmark rates. The administration’s plan includes a more stringent application of "risk adjustment" models—the mechanism used to pay insurers more for treating sicker patients. Critics of the current system, including fiscal hawks within the new administration, argue that insurers have engaged in "upcoding," or documenting more diagnoses than necessary to artificially inflate government payments. By implementing more rigorous audits and reducing the coding intensity adjustment, the government aims to claw back billions. For insurers, this represents a direct hit to the bottom line that cannot easily be offset by administrative cuts.
This fiscal hawkishness is part of a broader mandate led by the newly formed Department of Government Efficiency (DOGE), which has identified healthcare spending as a primary target for federal deficit reduction. With the US national debt exceeding $35 trillion and Medicare’s hospital insurance trust fund facing insolvency within the next decade, the administration is framing these cuts as an existential necessity. However, the timing is particularly precarious for insurers. The industry is already grappling with a "utilization spike"—a post-pandemic surge in elective surgeries and outpatient care among seniors—which has already compressed medical loss ratios (MLRs) across the board.
The economic implications of a leaner Medicare Advantage program extend far beyond the stock tickers of managed-care companies. If the government reduces the rates paid to insurers, those companies typically respond by either increasing premiums for seniors or, more likely, reducing the supplemental benefits that have made MA plans so popular. These benefits, which include dental, vision, hearing, and gym memberships, are not covered under traditional Medicare. A significant reduction in these "extras" could lead to a migration of beneficiaries back to the public system, potentially destabilizing the delicate public-private partnership that has defined senior care for twenty years.
Furthermore, the impact on the healthcare provider network could be substantial. Insurers squeezed by federal rate cuts often pass that pressure down to hospitals and physician groups through lower reimbursement rates or more frequent claim denials. This creates a secondary ripple effect across the economy, as health systems—already struggling with labor shortages and inflationary pressures—face their own margin contractions. Analysts suggest that the "Medicare squeeze" could accelerate the trend of hospital consolidations, as smaller, independent facilities find it impossible to survive on diminished payouts.
From a global perspective, the volatility in US healthcare stocks highlights the unique risks of a privatized entitlement system. In most other developed economies, such as those in Western Europe or East Asia, healthcare pricing is centrally negotiated and far more predictable, albeit often with lower ceilings on innovation and profit. The US model, which relies on market-based competition within a government-funded framework, offers higher potential returns but remains acutely sensitive to the shifting winds of political ideology. The current downturn underscores the "regulatory risk" that is inherent in any business model where the primary customer is the federal government.
Expert insights from the actuarial community suggest that the market may be reacting not just to the proposed cuts, but to the uncertainty of the implementation timeline. The Medicare Advantage "Rate Announcement," usually released in early spring, will be the first definitive test of the administration’s resolve. If the final rates are as low as the current rhetoric suggests, we may see a significant exit of insurers from certain rural or high-cost markets. This "geographic flight" could leave millions of seniors with fewer choices, a political outcome that the administration will have to balance against its cost-cutting ambitions.
Institutional investors are also closely monitoring the administration’s stance on the "Star Ratings" system. These ratings, which measure plan quality, determine a significant portion of the bonus payments insurers receive. Recent legal battles between insurers and the current CMS over rating methodologies have already injected volatility into the sector. A more punitive or transparently difficult rating system under the new administration would further erode the predictability of cash flows for companies like CVS Health, which has struggled to maintain high ratings for its Aetna-branded plans in recent cycles.
Despite the gloom on trading floors, some contrarian analysts argue that the sell-off may be overdone. They point out that the Trump administration has historically been a proponent of private-sector solutions and that Medicare Advantage remains a popular program with a powerful voting bloc: the elderly. There is a school of thought that the current rhetoric is a "negotiating opening" designed to force insurers to find efficiencies rather than a plan to dismantle the program entirely. If insurers can successfully lobby for a more moderate path, or if they can leverage artificial intelligence and value-based care models to lower their internal costs, the current low stock prices might eventually be seen as a generational buying opportunity.
However, the immediate reality remains one of defensive positioning. Portfolio managers are shifting capital out of pure-play insurers and into more diversified healthcare services or pharmaceutical companies that are less dependent on government capitation rates. The "Medicare Advantage gold rush" that defined the last decade appears to be over, replaced by a new era of fiscal austerity and regulatory scrutiny. As the transition team begins the process of installing new leadership at the Department of Health and Human Services (HHS), the industry is bracing for a period of protracted disruption.
The coming months will be a crucible for the US healthcare sector. The tension between the need for fiscal responsibility and the demand for high-quality senior care has never been higher. As the Trump administration moves from campaign promises to budgetary reality, the health insurance industry finds itself at a crossroads. The plummeting stock prices are a clear signal from the market: the era of easy growth in Medicare Advantage is ending, and the battle for the future of the American healthcare economy has begun in earnest. The resolution of this conflict will not only determine the fortunes of Wall Street giants but will also redefine the social contract for millions of American retirees for decades to come.