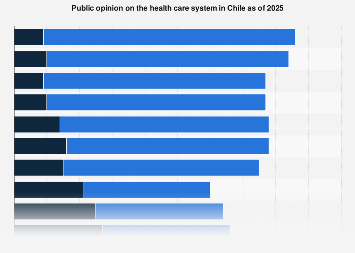
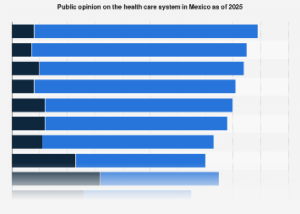
A significant portion of the Chilean populace harbors reservations about the efficacy and accessibility of their nation’s healthcare system, according to a comprehensive survey conducted in 2025. While approximately one-third of respondents expressed a degree of trust in the system’s capacity to deliver optimal medical treatment, this sentiment is tempered by widespread concerns regarding affordability and the timeliness of care. The findings paint a nuanced picture of a system grappling with public perception challenges, even as it endeavors to serve a diverse and growing population.
The survey data reveals a stark reality: nearly seven out of every ten individuals interviewed believe that a substantial segment of the Chilean population struggles to afford quality healthcare. This perception of inaccessibility is a critical indicator of systemic friction, suggesting that for many, the promise of good health remains financially out of reach. Such anxieties are not uncommon in many middle-income nations, where rapid economic development can sometimes outpace the expansion of social safety nets and equitable access to essential services. However, the intensity of this concern in Chile warrants closer examination of the underlying economic and structural factors at play. The implications extend beyond individual well-being, potentially impacting labor productivity, social mobility, and overall economic stability. When citizens fear they cannot afford to be sick, it creates a pervasive sense of insecurity that can ripple through the economy.
Compounding the affordability issue is the widespread perception of excessively long waiting times for medical appointments. Over six out of every ten respondents articulated this frustration, highlighting a bottleneck in the system that directly impedes timely medical intervention. In a world where preventative care and early diagnosis are increasingly recognized as crucial for positive health outcomes and cost containment, extended delays can lead to the exacerbation of conditions, increased healthcare expenditures in the long run, and a diminished quality of life for patients. This issue is particularly acute in urban centers, where population density often strains existing infrastructure, but can also be a significant problem in more remote areas where specialist access is already limited.
Despite these significant concerns, a notable segment of the Chilean population still views the quality of the healthcare system favorably. Around 23 percent of respondents characterized the quality as either good or very good. This suggests that while systemic issues related to access and affordability are prevalent, the actual delivery of medical services, particularly for those who can navigate the system, may be meeting certain standards. This dichotomy between perceived quality and accessibility underscores the complex nature of healthcare provision. It is possible that the positive experiences of some individuals, perhaps those with robust insurance coverage or who can access private facilities, are balanced against the struggles of a larger demographic facing financial or logistical hurdles.
Furthermore, the survey illuminated a trend towards individual agency in health decision-making. Approximately 35 percent of respondents indicated that individuals in Chile frequently take health decisions independently. This finding may reflect a growing awareness of personal health management, increased access to health information through digital channels, or a response to perceived shortcomings in the formal healthcare system. In an era of personalized medicine and increasing patient empowerment, this independent approach can be a positive development, fostering proactive health behaviors. However, it also raises questions about the role of healthcare professionals and the potential for misinformation if individuals are making critical health choices without adequate guidance or access to reliable medical advice. This trend could also be a consequence of the very issues identified – if people feel the system is slow or unaffordable, they may be more inclined to seek alternative solutions or manage their health proactively to avoid incurring costs or delays.
The Chilean healthcare landscape is a multifaceted entity, comprising a public sector funded through mandatory social security contributions and taxes, alongside a robust private sector. The public system, known as FONASA (Fondo Nacional de Salud), aims to provide universal coverage, while private health insurance plans, often referred to as ISAPREs (Instituciones de Salud Previsional), cater to a segment of the population seeking more comprehensive or specialized services. Historically, Chile has been lauded for its significant progress in improving health indicators over the past few decades, including increased life expectancy and reduced infant mortality rates. These achievements are often attributed to consistent public health policies and targeted interventions. However, the current survey data suggests that these gains may be facing headwinds, with public confidence showing signs of erosion.
Analyzing the economic implications of these perceptions is crucial. High out-of-pocket healthcare expenses can disproportionately affect lower-income households, widening the wealth gap and creating a cycle of poverty. When individuals are forced to choose between essential medical care and other basic needs, it can have devastating consequences for their long-term economic prospects and overall well-being. The World Health Organization consistently emphasizes that financial protection is a cornerstone of universal health coverage, and significant out-of-pocket spending is a key indicator of system vulnerability. Chile, like many emerging economies, is navigating the delicate balance between fostering economic growth and ensuring that the benefits of that growth are equitably distributed, particularly in critical sectors like healthcare.
The long waiting times also represent an economic drain. Delayed diagnoses can lead to more complex and expensive treatments down the line. Furthermore, a workforce that is frequently unwell due to delayed or inadequate care can result in decreased productivity, increased absenteeism, and a strain on social welfare systems. Businesses may face higher costs associated with employee health benefits and lost workdays. From a macroeconomic perspective, a population that is not healthy is a less productive population, which can hinder a nation’s overall economic competitiveness on the global stage.
Comparisons with other Latin American nations reveal that Chile’s challenges are not unique, but the specific combination of affordability concerns, access issues, and public trust levels offers a valuable case study. Countries like Costa Rica have often been cited for their strong public health systems and high levels of citizen satisfaction, though they also face their own unique demographic and resource challenges. Brazil, with its vast size and complex federal system, grapples with significant regional disparities in healthcare access and quality. Mexico’s healthcare system, a blend of public and private provision, also faces persistent issues with affordability and service delivery for large segments of its population. Chile’s situation, therefore, offers a lens through which to examine broader trends in healthcare reform and public policy across the region.
The trend towards independent health decision-making could also be interpreted as a signal that the existing healthcare infrastructure is not adequately meeting the perceived needs or expectations of the population. While individual empowerment is generally positive, it is essential to ensure that this autonomy is exercised within a framework of accessible and reliable medical expertise. Governments and healthcare providers alike have a responsibility to foster an environment where informed decisions can be made, supported by accessible consultations, clear communication, and equitable access to treatment options. This might involve investments in public health education, digital health platforms that provide reliable information, and more accessible channels for patient-physician interaction.
Looking ahead, addressing these concerns will likely require a multi-pronged approach. This could include policy interventions aimed at increasing affordability, such as expanding subsidies for low-income individuals, exploring price controls on pharmaceuticals, or strengthening primary care services to prevent the need for more costly interventions later on. Improving access could involve investments in healthcare infrastructure, particularly in underserved rural and peri-urban areas, as well as innovative solutions to reduce waiting times, such as telemedicine expansion, optimized appointment scheduling systems, and the increased utilization of allied health professionals. Building public trust will depend on consistent efforts to demonstrate transparency, accountability, and a genuine commitment to addressing the systemic challenges that are currently weighing on the minds of many Chileans. The future health and economic prosperity of Chile may well hinge on its ability to successfully navigate these complex and pressing healthcare issues.