The Drugs Controller General of India (DCGI) has issued a stringent directive to all pharmaceutical manufacturers and importers, demanding an immediate cessation of surrogate or indirect promotion of prescription drugs, with a particular focus on the burgeoning market for weight-loss and metabolic disorder medications. This decisive action, articulated in an advisory from the Central Drugs Standard Control Organization (CDSCO) on March 11, signifies a profound regulatory pivot aimed at safeguarding public health from potentially deceptive marketing strategies. The move comes as India grapples with a burgeoning obesity epidemic and the parallel rise of highly effective, yet complex, pharmaceutical interventions.
Authored by Rajeev Singh Raghuvanshi, India’s drugs controller general, the advisory underscores growing concerns that pharmaceutical entities have been leveraging subtle, often disguised, promotional avenues. These include strategic engagements on social media platforms, collaborations with influencers, and broader corporate awareness campaigns that, while appearing innocuous, are designed to create brand recall or product visibility for prescription-only medicines. Such practices are deemed a direct contravention of the Drugs and Cosmetics Act, 1940, and the Drugs Rules, 1945, which strictly prohibit the direct advertising of prescription medications to the general public in India. Unlike over-the-counter products like antacids or pain balms, which can be openly promoted, prescription drugs are meant to be prescribed by a qualified medical professional following a thorough diagnosis, making direct-to-consumer promotion ethically and legally problematic.
The advisory explicitly states that "Any form of advertisement, whether direct or indirect, which promotes prescription-only medicines to the general public, exaggerates therapeutic efficacy, suggests assured or guaranteed weight loss outcomes, downplays lifestyle modification measures (diet, exercise, behavioural interventions), or induces demand for pharmacological therapy, may amount to misleading promotion and may attract action under relevant provisions of the Drugs Rules, 1945, including principles underlying Schedule J of the said rules." This comprehensive language targets the very essence of indirect marketing, leaving little room for interpretation regarding what constitutes a violation. The emphasis on not undermining lifestyle interventions is crucial, as obesity is universally recognized as a chronic metabolic condition demanding a holistic management approach that prioritizes diet, physical activity, and behavioral modifications before, or in conjunction with, pharmacological therapy.
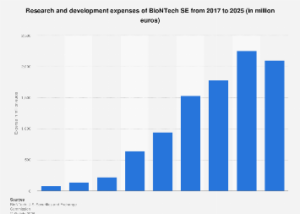
The global landscape for anti-obesity medications has been dramatically reshaped by the advent of GLP-1 receptor agonists, such as semaglutide and tirzepatide, marketed under various brand names like Ozempic, Wegovy, and Mounjaro. These drugs have demonstrated unprecedented efficacy in clinical trials for weight reduction and improving metabolic parameters, generating immense excitement among patients and healthcare providers alike. The global market for these drugs is projected to reach well over $100 billion by the end of the decade, reflecting their transformative potential. In India, while still nascent, the market for anti-obesity drugs is poised for explosive growth. The country faces a significant public health challenge, with national surveys like the National Family Health Survey (NFHS-5) indicating that approximately one in four adults (24% of women and 23% of men aged 15-49) are overweight or obese. This rising prevalence translates into an escalating burden of associated non-communicable diseases such as type 2 diabetes, cardiovascular disease, and certain cancers, placing immense pressure on the healthcare system and the national economy.
International pharmaceutical giants like Eli Lilly and Novo Nordisk, pioneers in the GLP-1 space, have already established a strong presence in the Indian market. Recognising the regulatory constraints against direct advertising, these firms have strategically launched multimedia awareness campaigns, often framed around "disease awareness" or "lifestyle improvement." While ostensibly educational, critics argue that such campaigns often subtly create an association with their specific drug classes or even brand names, thereby circumventing the spirit, if not the letter, of the law. This intensified marketing activity is further fueled by the impending patent expiry of semaglutide in India in early 2026, which is expected to unleash a wave of generic competition from domestic pharmaceutical companies. This impending rush for market share has amplified the urgency for regulatory clarity and enforcement.
Dr. Ambrish Mithal, Chairman of the Endocrinology Department at Max Hospital, Saket, Delhi, highlighted the dual nature of these medications. "The science behind these weight-loss drugs is very solid and they are extremely effective, as seen in extensive clinical trials, but they are not a ‘clean’ solution and can have potential side effects," he stated. "Because weight-loss is such an attractive proposition, we have seen a surge in popularity that likely drove the government to re-emphasize that these are not direct-to-public medications. They must only be used under the strict prescription and supervision of a trained doctor. I totally agree that there should be no element of advertising drugs directly to people; surrogate or direct promotion should be curtailed to ensure these treatments remain in a clinical setting where a doctor decides the best course of action." His comments underscore the ethical imperative of ensuring that powerful pharmacological therapies are prescribed responsibly, mitigating risks and optimizing patient outcomes.
The regulatory environment for prescription drug advertising varies significantly across major global markets. In the United States, Direct-to-Consumer (DTC) advertising for prescription drugs is permitted, albeit under strict regulations mandated by the Food and Drug Administration (FDA), requiring balanced information on benefits and risks. In contrast, most European Union member states and countries like Canada and Australia largely prohibit DTC advertising for prescription medicines, aligning more closely with India’s stance. These nations typically restrict promotional activities to healthcare professionals, emphasising medical education and professional detailing. India’s DCGI directive reinforces its position within this global framework, prioritising physician-led prescribing decisions over consumer demand generated by advertising.
Beyond merely prohibiting misleading promotions, the DCGI’s advisory introduces new measures aimed at bolstering transparency and accountability within the pharmaceutical sector. Manufacturers and marketing authorisation holders are now mandated to ensure that prescribing information and patient information leaflets for all prescription drugs clearly display the details of authorised officials, along with an official office code. Furthermore, these documents must provide a dedicated contact number and a complaint or ticket reference mechanism to facilitate consumer queries and streamline the reporting of adverse events or promotional concerns. These requirements are designed to empower consumers and healthcare professionals alike, ensuring that responsible personnel can be easily identified and held accountable. Additionally, all relevant parties are now required to submit a comprehensive risk management plan to the CDSCO, signalling a more proactive approach to pharmacovigilance and continued safety monitoring.
The CDSCO has also taken the crucial step of marking a copy of this advisory to the Advertising Standards Council of India (ASCI). The ASCI, a self-regulatory body for advertising content in India, plays a pivotal role in enforcing ethical advertising practices across various industries. This collaboration between the primary drug regulator and the advertising industry’s self-governing body is expected to foster a more unified and robust enforcement mechanism, ensuring industry-wide compliance and creating a deterrent against non-compliant marketing tactics.
The economic implications of this regulatory crackdown are significant. Pharmaceutical companies operating in India will need to re-evaluate their marketing strategies, shifting resources from broad-based awareness campaigns to more targeted engagement with healthcare professionals. This could involve increased investment in medical education, scientific symposia, and clinical detailing, which are permissible forms of communication with the medical fraternity. While this may initially impact the speed at which new products gain public recognition, it is likely to foster a more ethical and scientifically grounded approach to market development. In the long term, such measures can enhance public trust in the pharmaceutical industry and contribute to better public health outcomes by ensuring that advanced therapies are used appropriately and under expert guidance. The DCGI’s directive represents a critical juncture in India’s journey to balance innovation in pharmaceutical care with the paramount need for responsible, patient-centric healthcare promotion.