India’s Ministry of Health and Family Welfare, through its apex regulatory bodies, has initiated a sweeping overhaul of the nation’s blood transfusion infrastructure, implementing stringent new regulations designed to eradicate the pervasive issue of "professional donors" and replacement donation practices. This decisive action, spearheaded by the National Blood Transfusion Council (NBTC) and the Central Drugs Standard Control Organisation (CDSCO), marks a critical pivot towards establishing a 100% voluntary, non-remunerated blood donation system, aligning India with global best practices and fortifying public health safeguards. The move comes in the wake of disturbing incidents where children reportedly tested positive for HIV following blood transfusions, underscoring critical lapses in screening protocols in various states including Madhya Pradesh, Jharkhand, Rajasthan, and Assam.
The phenomenon of "professional donors" has long plagued India’s blood supply chain. These individuals, driven by financial incentives, often engage in frequent donations that exceed safe physiological limits, and may conceal high-risk behaviours or medical conditions, thereby significantly elevating the risk of transmitting infections such as HIV, Hepatitis B, Hepatitis C, syphilis, and malaria. The practice of "replacement donation," where patients’ families are pressured to provide a donor as a prerequisite for receiving blood, often inadvertently perpetuates this commercial cycle, pushing vulnerable individuals into selling their blood. The World Health Organization (WHO) consistently advocates for voluntary, unpaid blood donations as the cornerstone of a safe and sustainable blood supply, citing the lowest prevalence of transfusion-transmitted infections (TTIs) among such donor groups. Countries like the United Kingdom, the United States, and Japan have successfully transitioned to fully voluntary models, demonstrating the feasibility and profound benefits of such systems in ensuring a safer, more ethical, and efficient blood banking network.
Under the new directives, the eligibility criteria for establishing new blood banks and centres have been dramatically tightened. Only registered voluntary and charitable organizations with a proven track record of at least two years in healthcare delivery or blood transfusion services are now permitted to apply. Crucially, the regulations explicitly bar "family societies" or trusts, aiming to curb the proliferation of commercial entities disguised as non-profits. This measure seeks to dismantle the existing informal economy that thrives on paid donations, redirecting the focus from profit generation to public welfare. Prospective and existing blood centres are now mandated to undergo a rigorous social accountability evaluation, demonstrating their commitment to non-commercial practices through their Memorandum of Association and audited financial statements.

Operational and ethical benchmarks have been significantly elevated for both new and existing facilities. A key requirement is the establishment of in-house blood component separation and storage facilities within two years of receiving a license. This is a critical step towards modernizing blood banking, as component separation allows for more efficient utilization of donated blood (e.g., plasma, platelets, red blood cells), tailored to specific patient needs, thereby reducing wastage and maximizing therapeutic impact. Furthermore, blood banks are now required to submit an undertaking for an annual blood collection exceeding 2,000 units, with nearly 100% contribution from voluntary donors, preferably sourced through outdoor camps. To facilitate this, each blood bank must appoint a medical social worker and a counsellor dedicated to organizing voluntary donation drives and providing pre- and post-test counselling, emphasizing a holistic, patient-centric approach.
The economic implications of this regulatory shift are substantial. While the upfront investment for blood banks to meet new infrastructure requirements, particularly for component separation units, could be considerable, the long-term economic benefits are expected to outweigh these costs. The reduction in TTIs will significantly lower the burden on the public healthcare system, which currently incurs substantial expenses for treating complications arising from unsafe transfusions, including prolonged hospital stays, specialized medications, and managing chronic conditions like HIV and Hepatitis. Dr. K. Srinath Reddy, former president of the Public Health Foundation of India, highlighted this, stating, "Secure availability of blood to whoever needs it is an essential public health need. It is also absolutely essential that we ensure safety of the transfused blood, which must be free from infectious pathogens or toxic chemicals. Voluntarily donated blood, which is adequately tested, provides greater assurance of blood safety compared to paid donor blood."
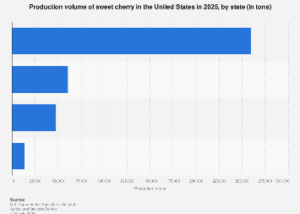
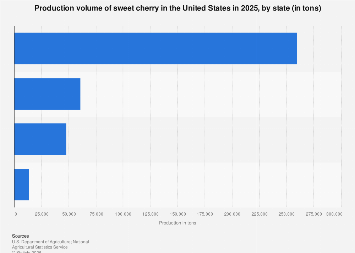
From a market perspective, the move towards 100% voluntary donation will necessitate a robust supply chain management system and enhanced public awareness campaigns. India currently requires an estimated 14.6 million units of blood annually, with the majority needed for medicine (41.2%), surgery (27.9%), and obstetrics/gynaecology (22.4%). The demand for specific blood types, such as O-negative and AB-positive plasma, remains consistently high. Shifting entirely away from paid donors requires a substantial increase in voluntary donor recruitment and retention. This presents both a challenge and an opportunity for non-governmental organizations and public health bodies to innovate in donor outreach and education. The emphasis on geographical distribution, mandating at least one blood bank per district while avoiding clustering in urban areas, also addresses the maldistribution of resources, ensuring equitable access to safe blood, especially in underserved rural and tribal regions.
A significant technological upgrade mandated by the government is the shift to fourth-generation enzyme-linked immunosorbent assay (ELISA) methods for screening donated blood, replacing less sensitive rapid card tests. This advanced diagnostic technology can detect viral loads at much lower levels, significantly enhancing the safety of the blood supply by reducing the "window period" during which infections might go undetected. This will likely drive demand for more sophisticated diagnostic kits and equipment, benefiting manufacturers in the medical technology sector.

The implementation of these reforms will not be without its challenges. Monitoring compliance across all 4,153 licensed blood banks and centres nationwide, particularly in remote and difficult terrains, will require robust regulatory oversight and adequate staffing for state blood transfusion councils (SBTCs). The transition period may see initial localized shortages as the informal supply channels are dismantled and the voluntary donation system scales up. However, the NBTC has shown pragmatism by allowing for relaxations in compliance requirements for rural, tribal, hilly, and desert regions, as well as for the armed forces, to ensure accessibility in difficult areas without compromising on the core principles of safety and ethics.
Ultimately, India’s regulatory overhaul signifies a critical commitment to public health and ethical practices within its healthcare system. By raising entry barriers, enforcing stringent operational standards, and promoting a culture of voluntary, non-remunerated donation, the government aims to forge a blood banking network that is not only safe and sufficient but also resilient and equitable. This strategic transformation is poised to have a lasting positive impact on the health and well-being of millions, safeguarding future generations from the risks associated with commercial blood donation. The long-term success will hinge on sustained public engagement, vigilant enforcement, and continuous adaptation to evolving medical science and societal needs.