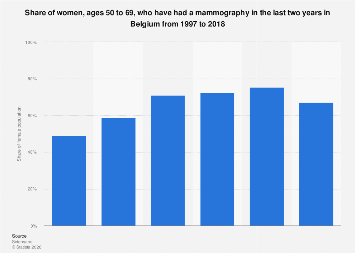
The landscape of breast cancer screening among Belgian women aged 50 to 69 has experienced notable shifts over a two-decade period, according to recent analyses of national health data. While the overall participation in mammography screenings has seen an upward trend for much of this timeframe, the most recent available data indicates a slight contraction in the prevalence of these vital early detection procedures. In 2018, approximately two-thirds of women within this age demographic reported having undergone a mammogram, a figure that, while substantial, represents a decrease from the peak participation levels observed in prior years. This nuanced pattern underscores the ongoing challenge of maintaining high and consistent engagement with preventative health services, even in well-established screening programs.
The historical data, tracing back to 1997, reveals a positive trajectory for mammography uptake in Belgium for women in the 50-69 age bracket. This period of growth can be attributed to a confluence of factors, including increased public awareness campaigns, the integration of screening into national healthcare frameworks, and advancements in mammography technology that have improved accuracy and accessibility. Early detection remains a cornerstone of effective breast cancer management, significantly improving treatment outcomes and survival rates. For every year that a woman in this age group skips a mammogram, her risk of a delayed diagnosis, and consequently a poorer prognosis, can increase.
However, the dip observed in 2018 warrants closer examination by public health officials and healthcare providers. Several potential contributing factors could explain this moderation. Economic conditions, changes in screening guidelines or recommendations, and even shifts in public perception or perceived necessity could play a role. Furthermore, the availability and accessibility of screening centers, particularly in rural or underserved areas, can impact participation rates. The statistical regression analysis used to extrapolate these figures, based on respondent demographics and the broader Belgian population in 2018, suggests that this trend is representative of the national picture, though it is important to acknowledge the methodology’s inherent estimations.
Globally, breast cancer screening participation rates vary significantly by country, influenced by differing healthcare systems, cultural norms, and public health investments. Countries with robust national screening programs, such as the United Kingdom or many Nordic nations, often report higher participation rates, frequently exceeding 70% and sometimes approaching 80% for their target age groups. In contrast, nations with less developed healthcare infrastructures or where screening is not universally subsidized may see considerably lower figures. Belgium’s position, with a majority of eligible women participating, places it within the upper tier of countries with established screening programs, but the recent decline highlights the need for continued vigilance and strategic intervention to sustain or improve these rates.
The economic implications of breast cancer screening are multifaceted. While there is an upfront cost associated with providing and accessing screening services, the long-term economic benefits of early detection are substantial. Identifying cancer at its earliest stages often leads to less aggressive and less costly treatments, reduced morbidity, and a quicker return to productivity for affected individuals. Conversely, delayed diagnoses can result in more complex and expensive treatment regimens, including surgery, chemotherapy, and radiation, along with prolonged periods of lost income and increased reliance on social support systems. Therefore, a slight decrease in screening participation, if it leads to an increase in late-stage diagnoses, could translate into higher healthcare expenditures and greater societal costs in the future.
To understand the 2018 figures more deeply, it is crucial to consider the nuances of the Belgian healthcare system. Belgium has a decentralized healthcare system with regional responsibilities, which could lead to variations in screening program implementation and outreach across Flanders, Wallonia, and Brussels. The effectiveness of regional public health campaigns, the density of mammography facilities, and the ease of appointment scheduling can all influence whether women adhere to recommended screening schedules. Moreover, factors such as socioeconomic status, educational attainment, and cultural background are known to correlate with health-seeking behaviors, including participation in cancer screenings.
The methodology employed in gathering these statistics, involving an online survey with a specific respondent pool of 1,569 women aged 50-69 in 2018, provides a valuable snapshot. However, reliance on online surveys can sometimes introduce a bias towards individuals who are more digitally connected and may not fully represent the entire demographic, particularly older individuals who are less likely to engage with online platforms. The statistical regression model, while attempting to account for broader population characteristics, is still an estimation. Future research could benefit from incorporating a wider range of data collection methods to capture a more comprehensive picture of screening behavior across all segments of the target population.
The trend of declining mammography prevalence in 2018, even if marginal, serves as a critical indicator for policymakers. It signals a potential need to re-evaluate and invigorate current public health strategies. This could involve targeted communication campaigns to remind women of the importance of regular screenings, addressing any identified barriers to access such as appointment availability or transportation, and ensuring that healthcare providers actively encourage and facilitate mammography appointments for their eligible patients. Collaborative efforts between government health agencies, medical associations, and patient advocacy groups are essential to reverse any downward trends and ensure that Belgian women continue to benefit from the life-saving advantages of early breast cancer detection. The long-term health and economic well-being of the population depend on maintaining high standards in preventative healthcare.