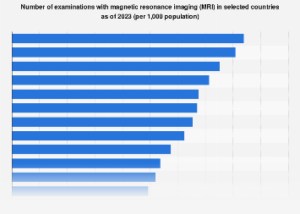
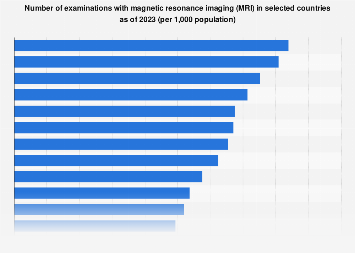
The global healthcare industry, a sector marked by relentless innovation and increasing demand, is profoundly shaped by the adoption and accessibility of advanced diagnostic technologies. Among these, Magnetic Resonance Imaging (MRI) stands as a cornerstone, offering unparalleled insights into the human body’s intricate structures without the use of ionizing radiation. As of 2023, a comprehensive analysis of MRI examinations across different nations reveals significant disparities in utilization, underscoring varying levels of healthcare infrastructure, economic capacity, and public health priorities. This examination delves into the factors influencing MRI accessibility worldwide, exploring the implications for patient care, medical research, and the broader economic landscape of healthcare.
The data indicates a stark contrast in MRI penetration rates globally. Developed economies, characterized by robust healthcare systems and substantial investment in medical technology, generally exhibit higher rates of MRI examinations per capita. Countries in North America and Western Europe, for instance, have long prioritized sophisticated diagnostic imaging, leading to widespread availability of MRI scanners and a correspondingly high volume of procedures. This saturation is often driven by a combination of factors including a higher prevalence of chronic diseases requiring detailed imaging, advanced medical research initiatives, and a healthcare reimbursement structure that supports the use of advanced diagnostics. For example, the United States, with its advanced healthcare infrastructure and significant private investment in medical technology, consistently ranks among the top in MRI procedure volume. Similarly, nations like Germany, the United Kingdom, and France, with their well-established public and private healthcare networks, demonstrate a strong commitment to providing accessible MRI services to their populations.
Conversely, many developing nations grapple with significant challenges in providing widespread access to MRI technology. Limited healthcare budgets, insufficient trained personnel, and the high cost of acquiring and maintaining MRI equipment often relegate these advanced diagnostic tools to a few specialized urban centers. This creates a pronounced urban-rural divide in healthcare access, where individuals in remote or underserved areas may have little to no access to MRI examinations, even when medically indicated. The economic burden of such advanced technology is a primary barrier. The acquisition cost of an MRI scanner can range from several hundred thousand to over a million U.S. dollars, a prohibitive expense for many healthcare systems in lower-income countries. Furthermore, the operational costs, including specialized maintenance, power consumption, and the need for highly trained radiographers and radiologists, add to the financial strain. This disparity not only impacts the timely diagnosis and treatment of diseases but also hinders medical research and the development of localized diagnostic protocols.
The economic implications of this global disparity are far-reaching. In countries with high MRI utilization, these procedures contribute significantly to the healthcare economy, supporting jobs in radiology, medical equipment manufacturing and servicing, and related administrative functions. Furthermore, early and accurate diagnosis facilitated by MRI can lead to more effective and less costly treatment interventions in the long run, potentially reducing the overall burden of disease and improving economic productivity. Conversely, in regions with limited access, delayed diagnoses can lead to more severe disease progression, requiring more complex and expensive treatments later on, or even resulting in permanent disability and reduced workforce participation. The investment in MRI technology, therefore, can be viewed not just as a healthcare expenditure but as a strategic investment in human capital and long-term economic development.
Several factors contribute to the observed differences in MRI utilization. The density of MRI scanners per million population is a key metric, but it only tells part of the story. The actual number of examinations performed is influenced by the prevalence of conditions that necessitate MRI, such as neurological disorders, orthopedic injuries, and certain cancers, as well as the healthcare policies that dictate referral patterns and reimbursement for diagnostic imaging. In countries with strong primary care systems and established pathways for specialist referrals, MRI utilization is likely to be more targeted and efficient. In contrast, systems with less structured referral processes might see either over-utilization or under-utilization depending on various factors.
Technological advancements are also playing a crucial role in shaping the global MRI landscape. Newer, more compact, and potentially lower-cost MRI systems are emerging, which could democratize access in resource-limited settings. Innovations in artificial intelligence (AI) are also being integrated into MRI workflows, aiming to improve image quality, reduce scan times, and automate certain aspects of image analysis. These advancements hold the promise of making MRI more accessible and efficient, potentially bridging some of the existing global gaps. However, the successful implementation of these technologies requires not only the hardware but also the digital infrastructure and skilled personnel to operate and maintain them.
The regulatory environment and healthcare financing models within each country also significantly impact MRI accessibility. Countries with universal healthcare coverage and policies that encourage preventive care and early diagnosis tend to have higher MRI utilization rates. Private healthcare markets, while often fostering rapid adoption of new technologies, can sometimes lead to disparities in access based on insurance coverage and out-of-pocket costs. Government subsidies, tax incentives for healthcare infrastructure development, and international aid programs can play a vital role in expanding MRI access in lower-income nations.
Looking ahead, efforts to improve global MRI accessibility will likely focus on a multi-pronged approach. This includes investing in training programs for radiographers and radiologists in underserved regions, exploring innovative financing models for equipment acquisition, and promoting the development and adoption of cost-effective MRI technologies. International collaboration and knowledge sharing between healthcare systems are also critical. By understanding the best practices and challenges faced by different countries, the global community can work towards a future where advanced diagnostic imaging like MRI is more equitably available, leading to improved health outcomes and a more robust global healthcare ecosystem. The 2023 data serves as a critical benchmark, highlighting both the progress made and the significant work that remains to ensure that the life-saving capabilities of MRI are accessible to all, regardless of their geographical location or economic standing.