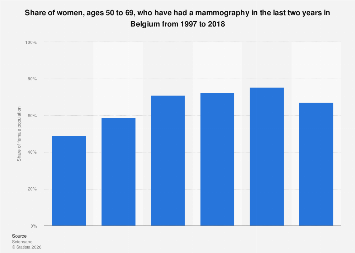
In 2018, approximately two-thirds of Belgian women between the ages of 50 and 69 reported undergoing mammography screenings, a key component of breast cancer early detection programs. This figure represents a significant segment of the population targeted by national health initiatives aimed at reducing breast cancer mortality. While the participation rate in these screenings has seen an upward trend since 1997, the most recent data from 2018 indicated a slight dip compared to the preceding period. This nuanced shift in screening prevalence warrants a closer examination of the factors influencing adherence and the broader implications for public health policy in Belgium and across Europe.
The landscape of cancer screening in developed nations is a complex interplay of public health campaigns, accessibility, individual health awareness, and evolving medical guidelines. Belgium’s experience with mammography screening for women over 50 offers a valuable case study in these dynamics. The long-term upward trajectory observed since the late 1990s suggests a growing awareness and acceptance of the benefits of regular mammograms. This period likely coincided with intensified public health messaging, improved accessibility to screening facilities, and perhaps a gradual increase in the proportion of women who perceive mammography as a vital tool for proactive health management. The initial growth phases of such programs are often characterized by a steady increase in uptake as awareness builds and screening becomes more integrated into routine healthcare.
However, the marginal decline recorded in 2018 introduces a layer of complexity. Several factors could contribute to such a plateau or slight decrease. These might include changes in the methodology of data collection, shifts in national screening guidelines or recommendations, economic pressures affecting healthcare access for some segments of the population, or a saturation point in participation for certain demographic groups. It is also possible that external events, such as public health crises or evolving public perception of medical interventions, could have played a role. Understanding the precise drivers behind this 2018 figure is crucial for policymakers to ensure that screening rates remain robust and continue to contribute effectively to breast cancer prevention and early diagnosis.
Globally, breast cancer remains a significant health concern, with incidence rates varying considerably by region and socioeconomic factors. In many European countries, organized mammography screening programs are a cornerstone of breast cancer control strategies. These programs typically target women within specific age brackets, usually between 50 and 69 years old, as this is the demographic with the highest incidence of breast cancer and where screening has demonstrated the greatest benefit in terms of reducing mortality. The European Union’s Council Recommendation on the early detection of cancer, for instance, encourages Member States to implement effective screening programs for breast cancer, emphasizing the importance of quality assurance and regular evaluation.
Comparing Belgium’s screening rates to those of its European neighbors provides further context. Countries like the Netherlands and the United Kingdom have historically reported high mammography screening participation rates, often exceeding 70% and sometimes reaching into the low 80s within their target populations. Nordic countries also typically exhibit strong participation, reflecting a strong tradition of public health investment and preventative care. Conversely, some Southern and Eastern European nations may face challenges in achieving comparable rates due to a variety of factors, including differences in healthcare infrastructure, funding priorities, and cultural attitudes towards preventative health measures. Belgium’s figures, hovering around the two-thirds mark, place it within the general range observed in many Western European countries, suggesting a solid but perhaps not fully optimized screening program.
The economic implications of mammography screening are substantial and multifaceted. On one hand, the direct costs associated with operating screening programs – including equipment, personnel, and logistical management – represent a significant public health expenditure. However, these costs are often offset by the considerable economic benefits derived from early cancer detection. When breast cancer is diagnosed at an early stage, treatment is typically less aggressive, less costly, and more effective. This leads to shorter treatment durations, reduced need for complex surgeries and prolonged therapies, and a quicker return to work for affected individuals. Consequently, early detection via mammography can lead to substantial savings in healthcare expenditures and a significant boost to economic productivity by minimizing the impact of the disease on the workforce.
Furthermore, the psychological and social benefits of early detection are immeasurable. Reducing the burden of advanced cancer on patients and their families not only improves quality of life but also lessens the strain on social support systems. The economic ripple effect extends to reduced disability claims, fewer long-term care needs, and sustained contributions to the economy by individuals who can continue their professional lives with minimal disruption. Investing in effective screening programs can therefore be viewed not merely as a health expenditure but as a strategic investment in human capital and long-term economic resilience.
The specific data points available from 1997 to 2018, while requiring specialized access for precise figures, indicate a clear pattern of growth in mammography screening participation among Belgian women aged 50-69. This period of over two decades saw the proportion of women availing themselves of this crucial health service steadily rise. The implied methodology, involving statistical regression based on survey responses, age, gender, and population data, suggests a robust effort to quantify this trend. The survey’s focus on women aged 50 to 69 is consistent with international best practices, as this age group represents a critical window for effective breast cancer screening.
The slight downturn in 2018, therefore, prompts deeper inquiry. Is this a temporary fluctuation, or does it signal a need for renewed efforts to engage the target population? Potential areas for investigation include examining regional variations in screening rates within Belgium, analyzing demographic subgroups that may be less engaged, and assessing the impact of recent public health campaigns or changes in the healthcare landscape. Understanding whether the decline is concentrated among specific age brackets within the 50-69 range, or if it reflects a broader societal trend, would be invaluable.
Moreover, the evolving landscape of breast cancer screening technologies and methodologies might also play a role. While mammography remains the gold standard for widespread screening, advancements such as tomosynthesis (3D mammography) and AI-assisted image analysis are increasingly being integrated into clinical practice. The awareness and adoption rates of these newer technologies, and their accessibility within national screening programs, could influence overall participation and perception of the screening process.
In conclusion, Belgium’s mammography screening rates for women over 50, while generally positive and showing long-term growth, experienced a subtle decline in 2018. This trend underscores the dynamic nature of public health initiatives and the need for continuous monitoring, evaluation, and adaptation. By delving into the specific factors contributing to this shift, drawing comparisons with international benchmarks, and analyzing the economic ramifications of screening, Belgium can further refine its strategies to ensure that this vital healthcare service continues to effectively protect the health and well-being of its female population, contributing to both individual prosperity and national economic vitality. The ongoing commitment to understanding and addressing the nuances of screening participation is paramount in the global fight against breast cancer.