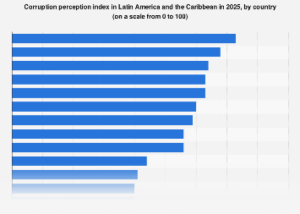
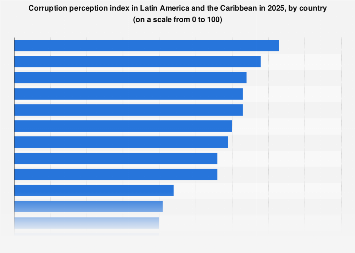
India stands at a critical juncture, grappling with a burgeoning public health crisis as the World Obesity Federation now ranks the nation as the third most obese globally, trailing only the United States and China. This alarming ascent from a historically lean population to a front-runner in the global obesity pandemic underscores a profound societal shift with far-reaching economic and healthcare implications. The urgency of this situation was emphatically highlighted by the Economic Survey 2026, which issued a stark warning regarding the accelerating prevalence of obesity across all age demographics, painting a concerning picture of national health and future productivity.
The scale of the challenge is further illuminated by a recent nationwide survey conducted by LocalCircles, revealing that a staggering three out of four Indians are acquainted with at least one obese individual within their close social fabric – encompassing family, friends, colleagues, or neighbours. This intimate proximity to the issue underscores its pervasive nature, transcending mere statistics to touch the daily lives of most citizens. A deeper dive into the survey’s findings reveals that 42% of respondents reported having four or more obese individuals in their immediate circle, indicating concentrated pockets of the health crisis. More critically, 56% observed that these obese individuals were concurrently battling lifestyle-related ailments such as diabetes, hypertension, high cholesterol, or fatty liver disease, illustrating the direct and severe comorbidities associated with excess weight.
The precipitous rise in obesity is not merely an isolated health concern but a symptom of profound changes in contemporary Indian society. The LocalCircles survey identified sedentary lifestyles, a dearth of physical activity, and the escalating consumption of fatty or ultra-processed foods as the primary drivers, with 64% of respondents attributing these factors to the obesity observed in their networks. This aligns perfectly with the Economic Survey’s diagnosis, which pinpointed unhealthy dietary patterns, increasingly sedentary routines, and the pervasive availability of highly processed food items as key contributors. Rapid urbanization, coupled with changing work cultures and easier access to convenience foods, has created an "obesogenic environment" where unhealthy choices are often the path of least resistance. The National Family Health Survey (NFHS-5) data further corroborates this trend, indicating that 24% of Indian women and 23% of men are now classified as overweight or obese. Disturbingly, this crisis is not sparing the youngest demographic, with childhood obesity among children under five years old escalating from 2.1% in 2015–16 to 3.4% in 2019–21, foreshadowing a generation potentially burdened with chronic diseases from an early age.
The economic ramifications of this escalating health crisis are substantial and multifaceted. Non-communicable diseases (NCDs), intrinsically linked to obesity, represent a colossal burden on India’s healthcare system and national economy. Conditions like Type 2 diabetes, cardiovascular diseases, certain cancers, and musculoskeletal disorders lead to increased medical expenditures for diagnosis, treatment, and long-term management. For individuals, this translates into out-of-pocket expenses that can deplete household savings and push families into poverty, particularly given the often-limited scope of health insurance in many segments of society. Public health systems, already stretched, face immense pressure to allocate resources towards managing these chronic conditions, potentially diverting funds from other critical public health initiatives. Economists estimate that the indirect costs, such as lost productivity due to illness, premature mortality, and absenteeism, could shave significant points off India’s potential GDP growth in the coming decades. A workforce battling chronic ailments is inherently less productive, impacting national competitiveness and innovation.
Globally, countries have adopted varying strategies to combat obesity, ranging from public awareness campaigns and nutritional education to fiscal interventions like "sugar taxes" or subsidies for healthy foods. Mexico and the UK, for instance, have implemented taxes on sugary drinks, while some Nordic countries have experimented with taxes on unhealthy fats. India’s challenge is uniquely complex, given its vast population, diverse dietary habits, and varying levels of socio-economic development. While pharmaceutical weight-loss solutions and bariatric surgeries are gaining traction among more affluent sections, health experts universally caution against viewing these as standalone panaceas. These interventions are often expensive, carry inherent risks, and fundamentally fail to address the underlying lifestyle and environmental factors driving the epidemic. The consensus among medical and public health professionals remains that sustainable lifestyle modifications—encompassing regular physical activity, balanced nutritional intake, and a significant reduction in ultra-processed food consumption—are the most effective and equitable long-term solutions.

Against this backdrop, the upcoming Union Budget 2026 is viewed by many as a pivotal moment for the government to articulate a robust and comprehensive strategy to tackle the obesity epidemic. Citizens, increasingly aware of the health and financial toll, are expressing clear expectations for policy interventions. A predominant demand from the LocalCircles survey respondents is for the government to introduce measures that enhance the affordability of products and services conducive to a healthy lifestyle. This includes reducing taxes on fitness-related activities, nutritious food options, and preventive healthcare services. Imagine a scenario where gym memberships, organic produce, or even basic sports equipment become more accessible through tax rebates or subsidies, thereby democratizing healthy living.
Beyond direct affordability, a multi-pronged policy approach within Budget 2026 could encompass several critical areas. Firstly, fiscal incentives could extend to businesses that promote employee wellness programs, offer healthy canteen options, or invest in on-site fitness facilities. Conversely, the government might consider implementing "fat taxes" on specific categories of ultra-processed foods, high-sugar beverages, and unhealthy snacks, similar to models adopted internationally. Revenue generated from such taxes could be ring-fenced to fund public health campaigns, nutritional education initiatives, or subsidies for fresh produce. Secondly, regulatory frameworks could be strengthened to mandate clearer nutritional labeling on food products, curbing deceptive marketing practices, especially those targeting children. Restrictions on advertising unhealthy foods during prime-time children’s programming or near schools could also be considered.
Thirdly, public health infrastructure and awareness campaigns require substantial investment. Budget 2026 could allocate funds for creating and maintaining public parks, walking trails, and cycling paths in urban and semi-urban areas, fostering an environment where physical activity is easily integrated into daily routines. School-based health and nutrition programs, including mandatory physical education and healthy meal options, are crucial for inculcating good habits from a young age. Mass media campaigns, leveraging popular figures and regional languages, could effectively disseminate information on balanced diets, the risks of sedentary living, and the benefits of regular exercise.
Moreover, the Budget could explore innovative partnerships with the private sector to develop affordable healthy food alternatives and expand their distribution channels, particularly in underserved areas. Support for local farmers engaged in sustainable, healthy food production could also be a focus, thereby strengthening the supply chain for nutritious options. Investment in research and development for nutritional science and behavioural economics, tailored to the Indian context, would also be invaluable in designing evidence-based interventions.
In essence, Budget 2026 presents an opportunity for India to pivot from a reactive healthcare model to a proactive, preventive public health strategy. Recognizing obesity not merely as an individual failing but as a societal challenge requiring systemic solutions is the first step. By strategically deploying fiscal measures, regulatory reforms, and public health investments, the government can play a transformative role in making healthier choices the easier choices for its citizens. This is not just about reducing the incidence of lifestyle diseases; it is about safeguarding India’s demographic dividend, enhancing its human capital, and ensuring sustainable economic growth for generations to come. The collective hope is that the upcoming budget will lay the foundation for a healthier, more productive India, preventing the need for costly medical interventions through timely and effective policy action.