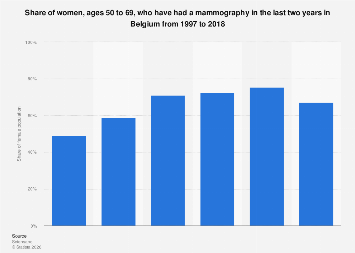
In 2018, a significant majority of Belgian women aged 50 to 69, approximately two-thirds, had undergone mammography screening. This figure represents a notable increase in participation compared to 1997, when the practice was less widespread. However, the data also indicates a slight dip in the prevalence of mammograms among this demographic in the most recent year surveyed, 2018. This trend underscores the dynamic nature of public health initiatives and the evolving landscape of preventative care within the Belgian healthcare system.
The evolution of breast cancer screening participation among Belgian women aged 50 to 69, spanning from 1997 to 2018, reveals a generally upward trajectory. This period coincides with increased global awareness campaigns and advancements in medical imaging technology, both of which are designed to encourage early detection of breast cancer. Early diagnosis is a critical factor in improving treatment outcomes and survival rates, making mammography a cornerstone of preventative health strategies for women in this age bracket. The Belgian government, like many European nations, has implemented national screening programs aimed at reaching a substantial portion of the target population. These programs typically involve regular invitations for screening, often subsidized or fully covered by public health insurance, to reduce financial barriers to access.
The slight decline observed in 2018 warrants further investigation. Several factors could contribute to such a phenomenon. These might include potential fluctuations in program outreach, public perception of screening efficacy, or even external events that may have temporarily impacted healthcare service utilization. Economic conditions can also play a role; while screening is often publicly funded, ancillary costs such as transportation or time off work can still pose challenges for some individuals. Furthermore, shifts in medical guidelines or evolving public health messaging could influence screening uptake. Understanding the precise reasons behind this minor contraction is crucial for maintaining and enhancing the effectiveness of future screening efforts.
Globally, breast cancer remains one of the most common cancers affecting women, and organized screening programs are a key strategy in managing its public health burden. Countries such as the United Kingdom, the Netherlands, and Sweden have long-established mammography screening programs with high participation rates, often exceeding 70% or even 80% among eligible women. These nations often serve as benchmarks for evaluating the success of screening initiatives. Belgium’s reported figures place it within a competitive range, demonstrating a commitment to women’s health. The European Union has set targets for screening participation, encouraging member states to achieve high coverage to maximize the impact of early detection on mortality rates.
The economic implications of effective breast cancer screening are substantial. Early detection through mammography can lead to less aggressive and less costly treatments, reducing the overall financial burden on individuals and the healthcare system. Studies have shown that the cost-effectiveness of mammography screening is highly dependent on achieving high participation rates. When screening is successful in identifying cancers at earlier stages, patients often require less intensive interventions, such as less extensive surgery, chemotherapy, or radiation therapy. This not only improves patient quality of life but also frees up healthcare resources that can be allocated to other critical medical needs. The long-term economic benefit extends beyond direct medical costs to include reduced loss of productivity due to illness and premature death.
The data collection methodology, as indicated by the survey details, involved an online survey with a specific number of respondents aged 50 to 69 in 2018, with a broader respondent pool for earlier years. The calculation of the share of the female population is noted to be based on statistical regression, accounting for age, gender, and the overall Belgian population in 2018. This statistical approach, while robust, suggests that the reported figures are estimates derived from a representative sample rather than a complete census. The reliability of such estimates is dependent on the quality of the sampling and the accuracy of the regression models employed.
Looking ahead, the focus for Belgium, and indeed for public health bodies worldwide, will be on understanding and addressing any factors contributing to a plateau or decline in screening rates. This could involve enhanced public awareness campaigns tailored to specific demographic groups, improved accessibility of screening facilities, and continuous evaluation of the screening program’s operational efficiency. Technological advancements, such as digital mammography and artificial intelligence for image analysis, are also poised to play a role in improving the accuracy and efficiency of screening. Furthermore, a more granular analysis of the 2018 dip could reveal insights into regional disparities or specific sub-groups within the 50-69 age bracket that require targeted interventions. Sustaining and ideally increasing mammography screening participation is paramount to realizing the full public health benefits of early breast cancer detection in Belgium. The long-term success of these programs hinges on a sustained commitment to monitoring trends, adapting strategies, and ensuring equitable access for all eligible women.