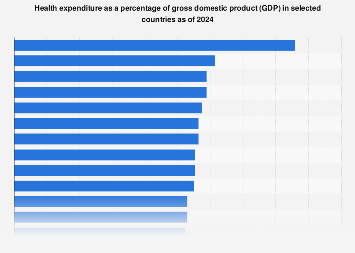
In 2024, the United States stands out among its Organization for Economic Co-operation and Development (OECD) peers for allocating the largest portion of its gross domestic product (GDP) to healthcare. Preliminary data indicates that the U.S. devoted nearly [Insert specific percentage here, e.g., 17.3%] of its economic output to healthcare services, a figure significantly higher than other industrialized nations. Following the U.S. in healthcare spending as a percentage of GDP, though at considerably lower rates, were countries such as Germany and Austria, alongside other OECD members. This pronounced difference underscores the substantial investment the United States makes in its healthcare infrastructure and services, encompassing both public and private expenditures, compared to other developed economies.
The rationale for focusing on OECD countries in such comparisons is rooted in their shared commitment to developed economies, advanced industrialization, and generally high standards of living. These nations often represent a benchmark for policy development and economic analysis, providing a context for understanding national spending patterns. By examining healthcare expenditure as a proportion of GDP within this group, policymakers, economists, and researchers can identify trends, assess the efficiency of healthcare systems, and gauge the fiscal pressures that such spending exerts on national economies. The OECD, comprising 38 member countries, offers a valuable dataset for cross-national analysis of economic and social policies.
The divergence in healthcare spending as a percentage of GDP among OECD nations can be attributed to a complex interplay of factors. These include the structure of healthcare financing (e.g., single-payer systems versus multi-payer private insurance models), the comprehensiveness of publicly funded services, the prevalence of chronic diseases and an aging population, the cost of medical technologies and pharmaceuticals, administrative overhead, and the overall efficiency of healthcare delivery. The U.S. system, characterized by a significant private insurance component, high pharmaceutical prices, and a fee-for-service reimbursement model in many areas, has historically driven up per capita and GDP-percentage spending.
For instance, in 2022, U.S. per capita healthcare spending was estimated to be around [Insert specific figure, e.g., $12,555], dramatically exceeding the averages of other high-income countries. This high per capita spending, when translated into a percentage of GDP, reflects a national economy that dedicates a substantial share of its resources to the health and well-being of its population. While this level of investment can translate into access to advanced medical treatments and cutting-edge research, it also raises questions about affordability, equity, and the sustainability of such expenditure in the long term.
The economic implications of high healthcare spending are multifaceted. On one hand, the healthcare sector itself is a significant employer and contributor to economic activity, driving innovation and demand for goods and services. Investment in health can also lead to a more productive workforce, as healthier individuals are generally more capable of participating in the labor market. However, a disproportionately large share of GDP allocated to healthcare can potentially crowd out other essential public services, such as education, infrastructure, or defense, and may also place a considerable burden on taxpayers and private consumers through insurance premiums and out-of-pocket costs.
Looking at the broader global landscape, while the OECD countries offer a valuable comparison group, it is important to acknowledge that healthcare spending patterns vary widely across the world. Developing economies, for example, often face different challenges, with lower overall GDP and a greater proportion of their populations lacking access to basic healthcare services. Their healthcare expenditure as a percentage of GDP may appear lower, but this often reflects underinvestment rather than systemic efficiency. International organizations like the World Health Organization (WHO) track global health expenditure, providing a wider lens on how different countries prioritize health.
The trend of rising healthcare costs is a global phenomenon, exacerbated by factors such as the increasing burden of non-communicable diseases, the development of expensive new medical technologies, and the growing demand for healthcare services from an aging global population. Even countries with more centralized or publicly funded healthcare systems are grappling with the challenge of controlling costs while ensuring quality and access. This makes the U.S. experience, while extreme in its current manifestation, a bellwether for discussions on healthcare reform and fiscal responsibility worldwide.
Furthermore, the specific components of healthcare spending – such as administrative costs, pharmaceutical expenses, and hospital services – often differ significantly between countries. For example, the U.S. system’s reliance on private insurers leads to higher administrative overhead compared to single-payer systems where administrative functions are more streamlined. Similarly, the pricing of prescription drugs in the U.S. is often higher than in countries where governments negotiate prices on behalf of their entire population. Understanding these granular differences is crucial for a comprehensive analysis of why certain nations spend more on healthcare than others.
In conclusion, the United States’ position as the highest spender on healthcare as a percentage of GDP among OECD nations in 2024 is a significant economic indicator. It highlights a nation that prioritizes healthcare investment, albeit with considerable debate surrounding its efficiency, equity, and long-term sustainability. The comparative data from other developed nations provides a vital benchmark for understanding the various approaches to healthcare financing and delivery, offering valuable insights for policymakers grappling with the universal challenge of providing quality healthcare within fiscal constraints. The ongoing evolution of healthcare systems globally ensures that this metric will remain a critical point of analysis for years to come.