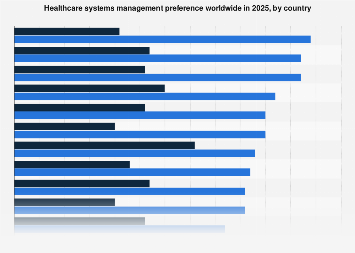
The year 2025 finds healthcare systems worldwide at a critical juncture, grappling with unprecedented demographic shifts, rapidly advancing medical technologies, and the enduring imperative to deliver equitable and sustainable care. As nations continue to refine their approaches to healthcare governance, a prevailing consensus is emerging around specific management frameworks, with a discernible global preference for models that prioritize integrated care, patient-centricity, and data-driven decision-making. This evolving landscape reflects a broader trend in global economics, where efficiency, adaptability, and stakeholder alignment are paramount for success.
Historically, healthcare management has been a complex tapestry of public, private, and mixed models, each with its own strengths and weaknesses. The traditional fee-for-service model, while driving innovation in some areas, has increasingly been criticized for its potential to inflate costs and create fragmented patient journeys. In response, many countries are actively migrating towards value-based care paradigms, where providers are incentivized not just by the volume of services rendered, but by the quality of outcomes achieved and the overall health of the populations they serve. This shift is particularly pronounced in developed economies with aging populations and a rising burden of chronic diseases, such as the United States, the United Kingdom, and Canada. For instance, initiatives like the Accountable Care Organizations (ACOs) in the U.S. aim to foster collaboration among healthcare providers to coordinate care for Medicare beneficiaries, thereby improving the quality of care and reducing unnecessary costs. Similarly, the UK’s National Health Service (NHS) continues to explore integrated care systems, seeking to break down traditional silos between primary, secondary, and social care services.
The rise of digital health and artificial intelligence is also profoundly reshaping healthcare management strategies. The ability to collect, analyze, and act upon vast amounts of patient data offers unparalleled opportunities for proactive disease management, personalized treatment plans, and operational optimization. Countries that have invested heavily in digital infrastructure and data interoperability, such as Estonia and Singapore, are at the forefront of leveraging these technologies. Estonia’s e-health system, for example, allows for seamless sharing of patient records among authorized healthcare professionals, enhancing care coordination and reducing medical errors. Singapore’s HealthTech initiatives are focused on utilizing AI for diagnostics, drug discovery, and predictive analytics to anticipate disease outbreaks and manage population health. The economic implications of this digital transformation are substantial, promising not only improved patient outcomes but also significant cost savings through increased efficiency and reduced waste. A report by the World Economic Forum projected that digital health could unlock trillions of dollars in economic value globally by 2030.
However, the implementation of these advanced management models is not without its challenges. Data privacy and security remain paramount concerns, requiring robust regulatory frameworks and technological safeguards. The digital divide, which exacerbates inequalities in access to technology and digital literacy, also poses a significant hurdle, particularly in lower-income countries. Furthermore, the transition to value-based care demands a fundamental shift in organizational culture and workforce training, requiring healthcare professionals to embrace new collaborative approaches and data-analytic skills. The International Monetary Fund (IMF) has highlighted the importance of investing in human capital and digital infrastructure as key enablers for successful healthcare reforms.
Emerging economies are also actively seeking to optimize their healthcare management. Countries like India and Brazil, with their large and diverse populations, are experimenting with innovative public-private partnerships and community-based healthcare delivery models. The focus in these regions is often on expanding access to basic healthcare services, improving maternal and child health, and combating infectious diseases, while simultaneously building the capacity for more complex care. The adoption of mobile health (mHealth) solutions, for instance, has proven to be a cost-effective way to reach remote populations and provide essential health information and services. Initiatives like India’s National Health Mission, which aims to provide accessible, affordable, and quality healthcare to all citizens, are increasingly incorporating digital tools and integrated care approaches.
The global pharmaceutical and medical device industries are intrinsically linked to these management trends. As healthcare systems shift towards value-based outcomes, there is a growing demand for innovative therapies and technologies that demonstrate clear clinical and economic benefits. This is driving increased investment in research and development focused on precision medicine, targeted therapies, and minimally invasive surgical techniques. Companies that can provide evidence of improved patient outcomes and cost-effectiveness are likely to gain a competitive advantage. The market for personalized medicine, for example, is projected to grow significantly in the coming years, reflecting a broader move away from one-size-fits-all approaches.
Looking ahead, the management of healthcare systems in 2025 and beyond will likely be characterized by a dynamic interplay of technological innovation, evolving patient expectations, and the persistent need for fiscal responsibility. The models that prove most resilient and effective will be those that can foster collaboration across sectors, empower patients as active participants in their own care, and harness the power of data to drive continuous improvement. The global pursuit of efficient, equitable, and high-quality healthcare remains a defining challenge of our time, with significant implications for individual well-being and overall economic prosperity. The ongoing evolution of management strategies worldwide offers a hopeful outlook for addressing these complex issues, albeit with a recognition that the journey requires sustained commitment and adaptive leadership.